Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Amy Choi, Medical Registrar, Waikato Hospital, Hamilton, New Zealand. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. January 2020.
Introduction Demographics Causes Clinical features Diagnosis Differential diagnoses Treatment Outcome
Reactive arthropathy describes the inflammation of joints following an infection usually involving the gastrointestinal or urogenital tracts [1–3]. Symptoms of arthritis typically begin a few weeks after the initial infection and may persist for several months to a year. Microorganisms cannot be cultured from the joints in reactive arthropathy as the infection occurs elsewhere in the body, distinguishing this from septic arthritis [3].
Reactive arthropathy is also known as reactive arthritis. The triad of reactive arthropathy associated with inflammation of the bladder outflow tract (urethritis) and the eyes (conjunctivitis) was formerly termed Reiter disease or Reiter syndrome [2] and is commonly associated with mucocutaneous changes.
Reactive arthropathy may also be associated with skin changes and lesions of the mucous membranes [3].
Reactive arthropathy affects both men and women and is seen most commonly in young adults between the ages of 20 and 40 years [1].
In the Caucasian population, HLA-B27 antigen and HIV/AIDS are strongly associated with reactive arthropathy [1,3,4].
Reactive arthropathy is triggered by an infection of the urogenital or gastrointestinal tracts. Cross-reactivity of the immune system between infectious antigens and self-proteins is thought to result in an autoimmune response [3].
Typical pathogens affecting the gastrointestinal tract include:
Pathogens affecting the genitourinary tract include:
The underlying infection may be asymptomatic, particularly in women.
The inability to culture a typical pathogen does not exclude the diagnosis of reactive arthropathy. In up to 40% of patients, no infectious organism is found [2].
Patients may report symptoms of a recent systemic infection, particularly involving the genitourinary or gastrointestinal tract. These typically precede musculoskeletal symptoms by several days to a few weeks and include:
Clinical features of the reactive arthropathy are similar regardless of the precipitating infection.
Common ocular symptoms include pain, redness and irritation of the eyes (conjunctivitis). In some cases, uveitis and iritis may occur, causing blurred vision, light sensitivity and headaches [1,3].
Cardiac symptoms include heart valve abnormalities and abnormal electrical activity. Kidney and central nervous system involvement are rare [3].
Skin involvement develops some months after the onset of arthritis. Cutaneous signs include:
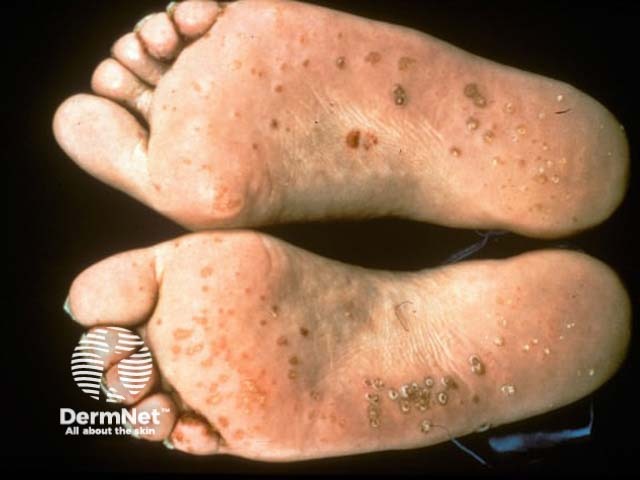
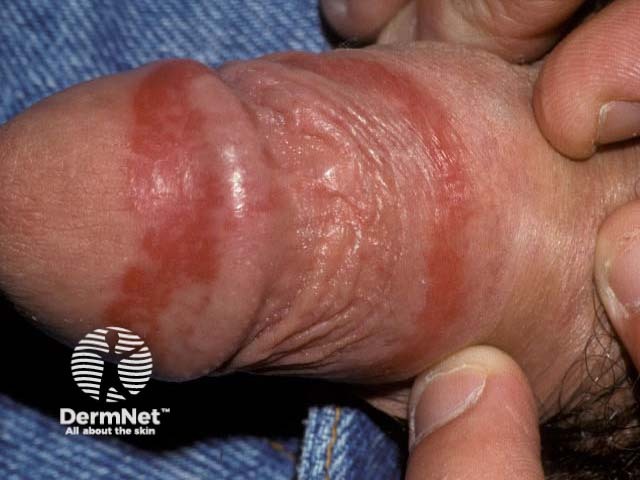
Reiter syndrome

Erythema nodosum
A diagnosis of reactive arthropathy is based on the pattern of symptoms and signs. Although there are no specific tests to confirm the diagnosis of reactive arthropathy, it may be suspected when the following key features are present and other causes for the symptoms have been excluded [1]:
Samples of fluid may be taken from swollen joints using a needle (arthrocentesis) to culture for the presence of microorganisms (found in septic arthritis) or to examine under microscopy for crystals (found in gout or pseudogout) [5].
Plain film x-rays may be performed to rule out other causes for joint pain [1]. Ultrasound scans and magnetic resonance imaging (MRI) may be useful to demonstrate musculoskeletal inflammation [5].
HLA-B27 and HIV testing are recommended.
The diagnosis of reactive arthropathy requires that other causes of joint pain and swelling are excluded. This includes both infective and inflammatory processes.
Antibiotics should be initiated to reduce the risk of progression or complications from the initial infection. This is particularly important for genitourinary infections such as chlamydia [2]. Antibiotics have not been shown to affect the outcome of the reactive arthropathy [5].
Pain, joint swelling, and reduced mobility are treated with:
While these treatments may provide relief from the symptoms of reactive arthropathy they do not shorten the duration of disease. DMARDs are often introduced for persistent symptoms lasting more than 3–6 months to avoid the side effects of long-term prednisone.
Patients with suspected eye involvement should be assessed by an ophthalmologist for further management.
Treatment of the cutaneous disease associated with reactive arthropathy is like the treatment of psoriasis.
Reactive arthropathy is usually a self-limited condition and carries a good prognosis. Symptoms typically persist for several months then resolve completely. A few people develop chronic arthritis with ongoing symptoms for longer than one year. These patients are more likely to be HLA-B27 positive [2,5].