Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Introduction - diagnoses of urticaria
Introduction - urticaria
Ordinary urticaria
Urticaria-like skin lesions
Urticaria associated with systemic disease
This topic provides a differential diagnosis for urticaria and for urticaria-like conditions that resemble urticaria but are not caused by wealing.
Urticaria describes a group of conditions in which there are weals (or weals) in the skin, itchy white or red lumps. Urticaria can occasionally be a sign of systemic disease.
Spontaneous or 'ordinary' urticaria is divided into acute urticaria (lasting a few hours or days or up to six weeks) and chronic urticaria (persisting more than six weeks, and sometimes life-long).
The weals are well defined raised lesions with a smooth surface. They may be red or white, surrounded by a red or white flare. Weals range in size from a few millimetres to many centimetres in diameter. The shape also varies: round, polycyclic (overlapping circles), annular (ring-shaped), geographic (like a map). They are randomly distributed on the body and may affect any site. They last no more than 24 hours and do not leave any marks behind.
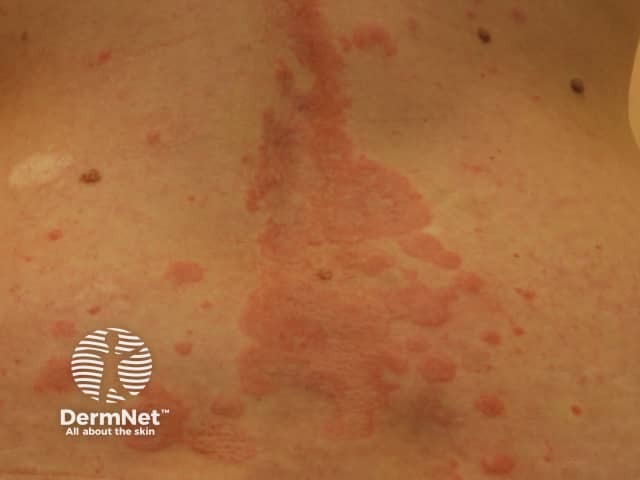
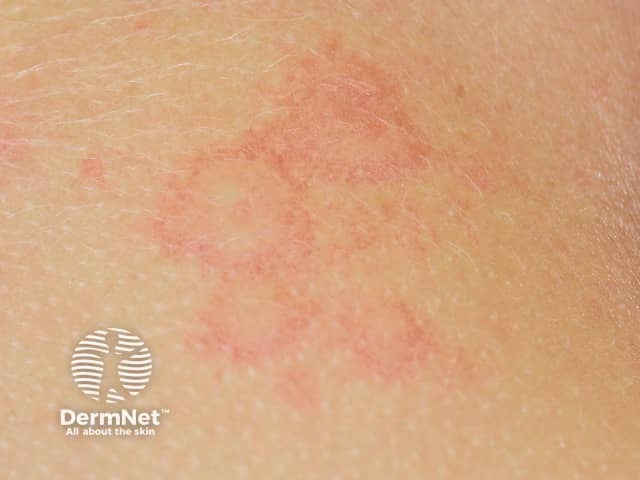
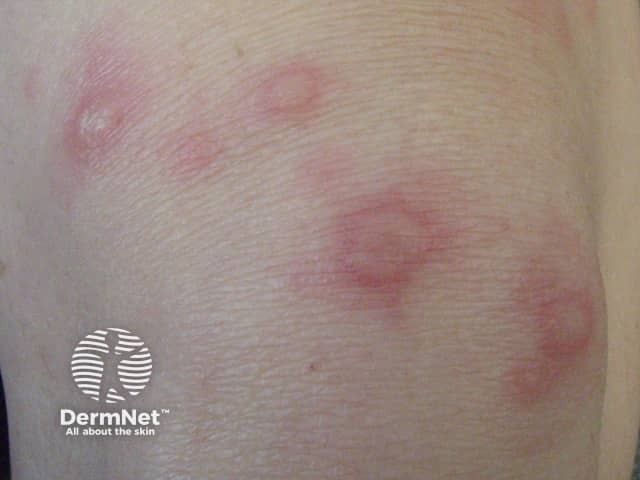
See more about ordinary urticaria.
Chronic inducible urticaria (previously known as physical urticaria) arises in response to an external factor. Classification is according to the provoking factor: stroking the skin in dermographism (skin writing), acetylcholine released during sweating in cholinergic urticaria, cold air or water in cold urticaria, local heat in heat urticaria, a contact factor in contact urticaria, water of any type or temperature in aquagenic urticaria, sun exposure in solar urticaria and firm pressure in delayed pressure urticaria. Physical urticarias have the following characteristics.

Dermographism
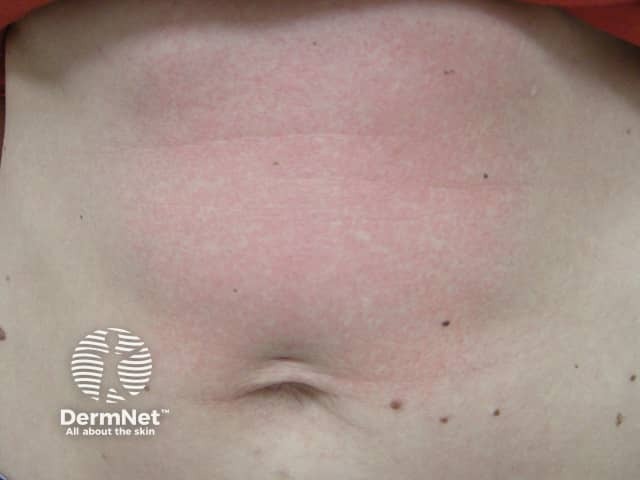
Solar urticaria provoked experimentally
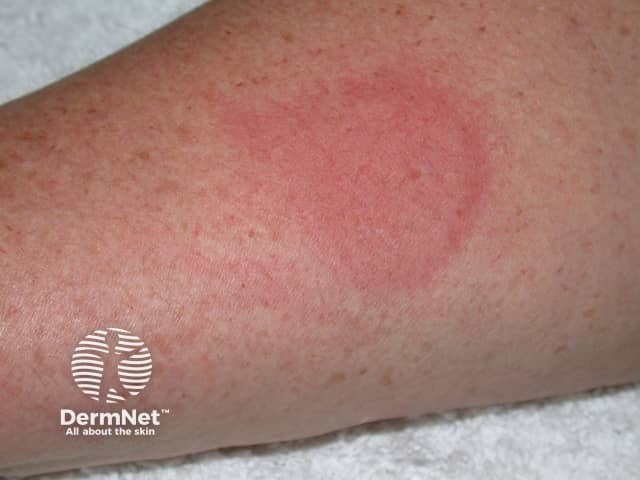
Cold urticaria provoked by ice cube
Urticaria-like skin lesions are reddish or skin-coloured flat patches or swellings with a smooth surface that persist for more than 24 hours.
Insect bites often result in itchy bumps (papules) or weals. Their characteristics include:
Children and, less frequently, adults may develop papular urticaria, which is interpreted as a hypersensitivity reaction to insect bites. No initial sting is felt, and old lesions may reappear.
A biopsy reveals an inflammatory infiltrate that includes eosinophils and spongiosis of the epidermis.
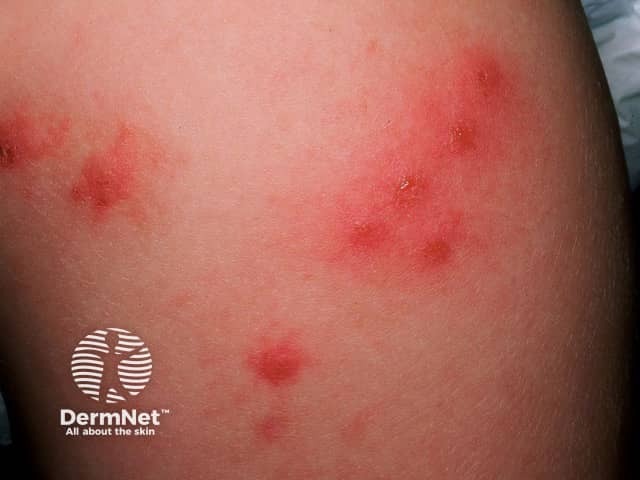
Insect bites
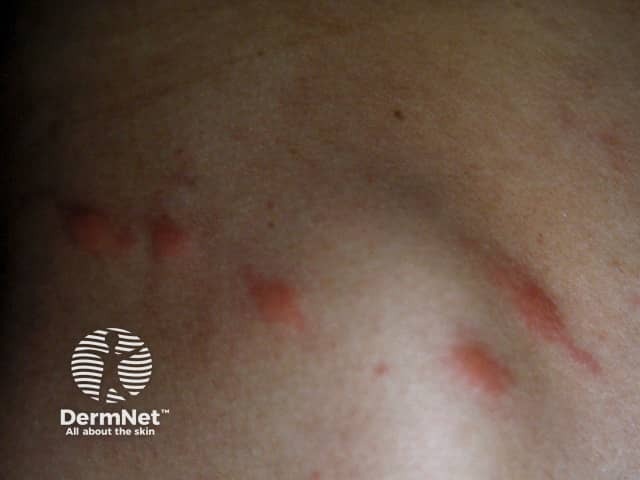
Insect bites
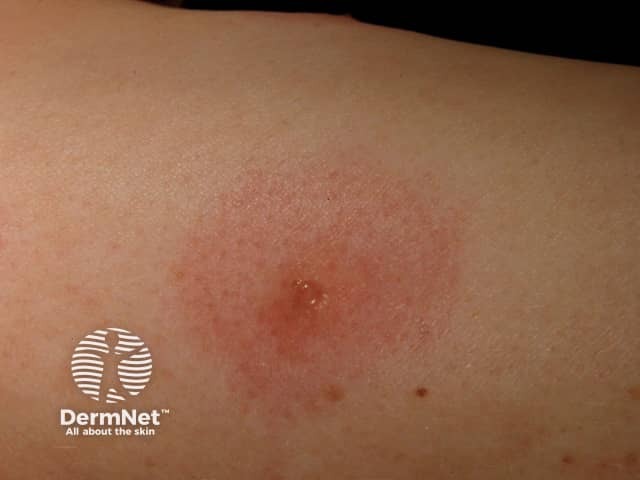
Insect bites
Urticarial dermatitis presents with both urticaria-like and eczema-like lesions.
A biopsy may be reported as dermal dermatitis with mixed inflammatory cells in the dermis and minimal spongiosis in the epidermis.
Urticarial dermatitis can be an early sign of bullous pemphigoid. Eventually, tense blisters appear. Biopsy features eosinophils and subepidermal clefting with positive staining on direct immunofluorescence.

Urticarial dermatitis
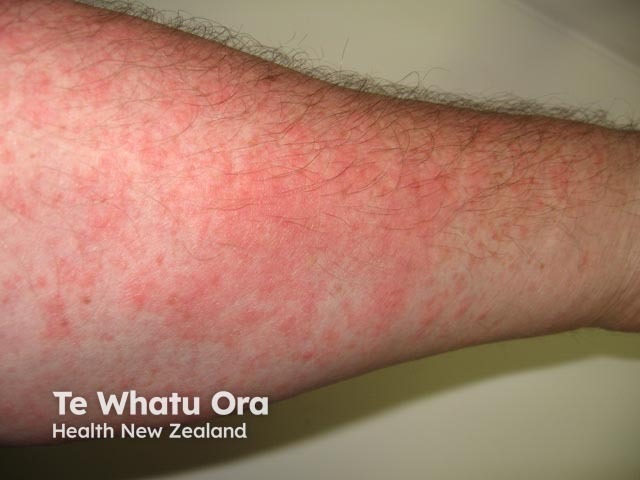
Urticarial dermatitis

Urticarial dermatitis
Contact dermatitis sometimes appears urticarial rather than eczematous, with most of the inflammation in the dermis rather than the more superficial epidermis.
Contact dermatitis should be distinguished from contact urticaria, which is a short-lasting type of physical urticaria (see above).
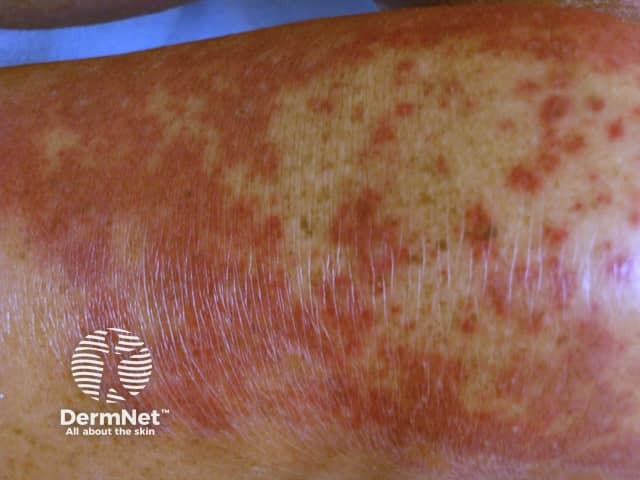
Dermal contact dermatitis
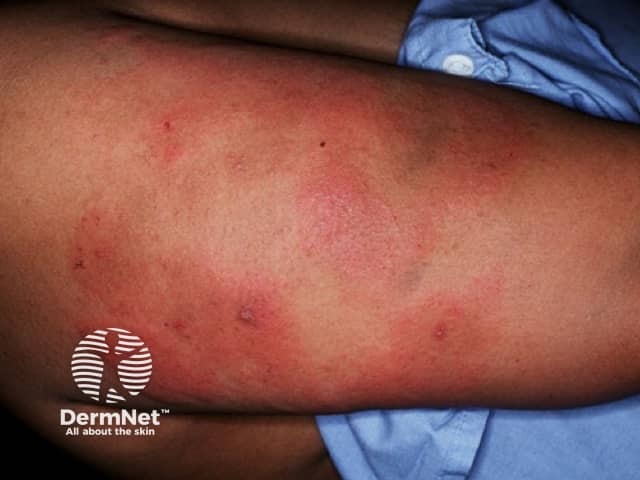
Dermal contact dermatitis
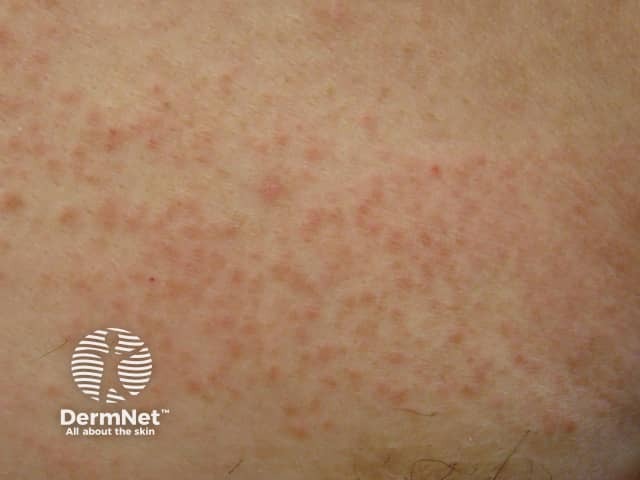
Dermal contact dermatitis
Classic erythema multiforme presents with an acute eruption of target-shaped lesions on the hands, feet, knees and elbows. However target-shaped lesions may also be seen in ordinary urticaria.
A biopsy is usually characteristic.
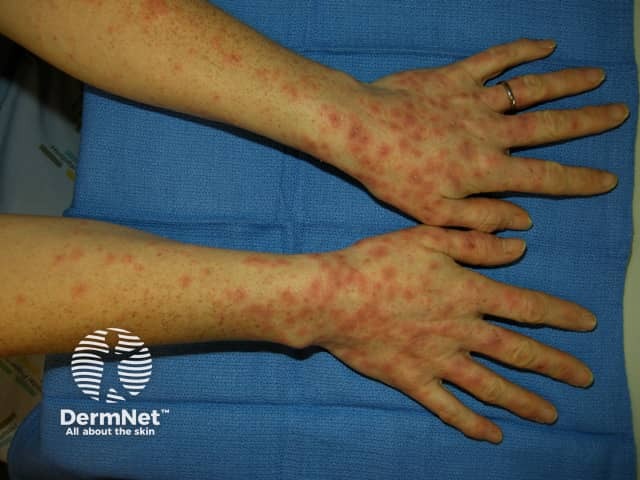
Erythema multiforme

Erythema multiforme
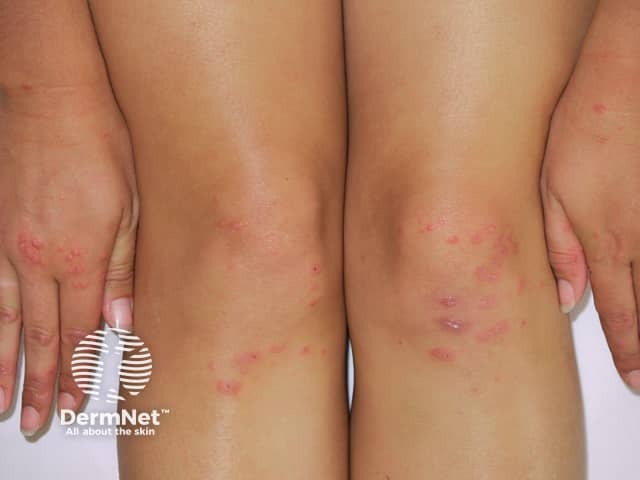
Erythema multiforme
Drug eruptions include urticaria and urticaria-like eruptions. Individual lesions resolve within hours in drug-induced urticaria and persist for days in urticaria-like eruptions. They are often described as morbilliform or maculopapular eruptions. Characteristics of drug eruptions include:
A biopsy reveals a subtle inflammatory infiltrate that includes eosinophils, and lymphocytes and apoptotic keratinocytes in the epidermis.
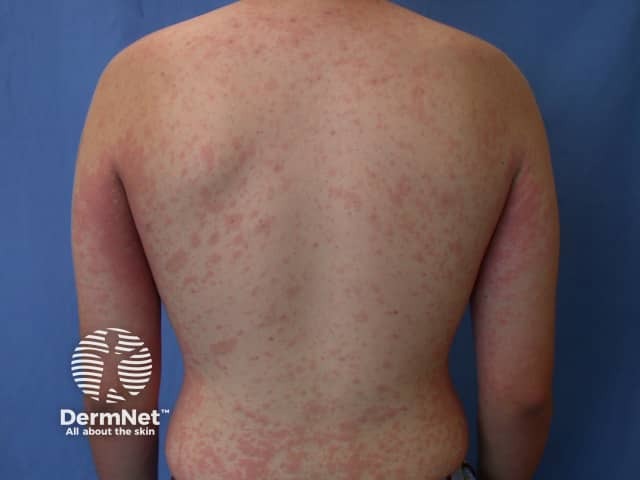
Drug eruption
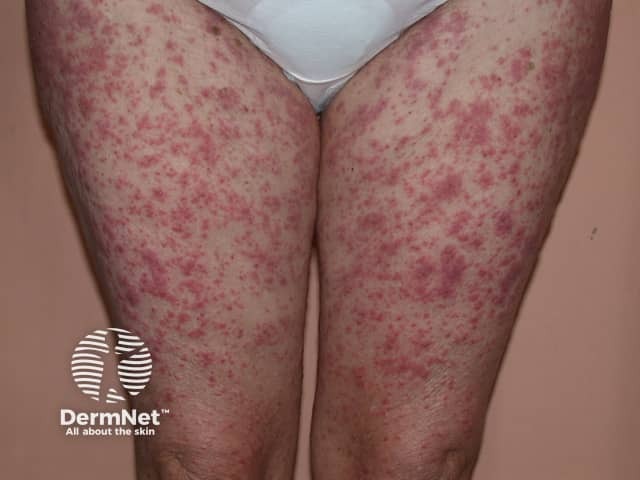
Drug eruption
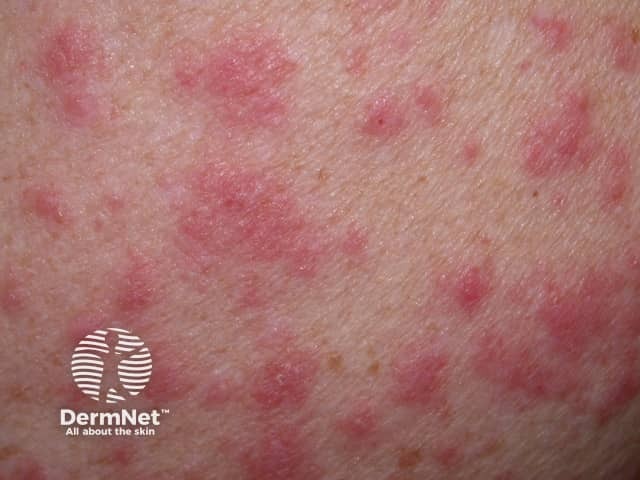
Drug eruption
Urticaria pigmentosa is a form of cutaneous mastocytosis in which there are brown macules and papules.
A biopsy may reveal increased numbers of mast cells, but these can be difficult to identify, and the tissue may look the same as normal skin.
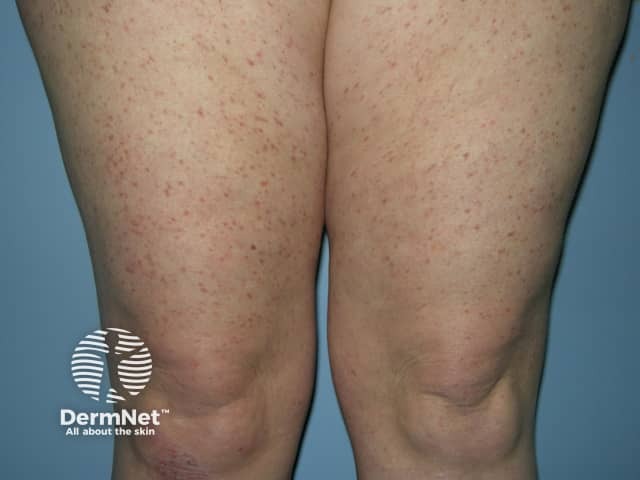
Urticaria pigmentosa: brown spots that urticate
The subepidermal autoimmune blistering diseases may initially present with urticarial lesions several days or weeks before blisters appear. These urticarial lesions may be seen in:
The characteristics of autoimmune blistering diseases include:
Skin biopsy for routine histopathology and direct immunofluorescence studies are necessary to confirm the diagnosis.
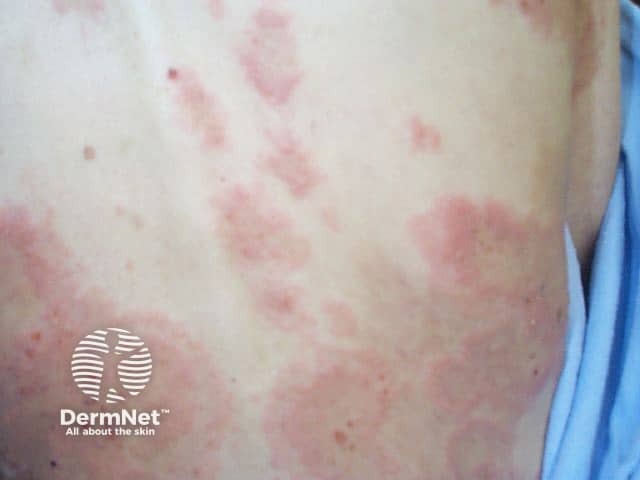
Bullous pemphigoid
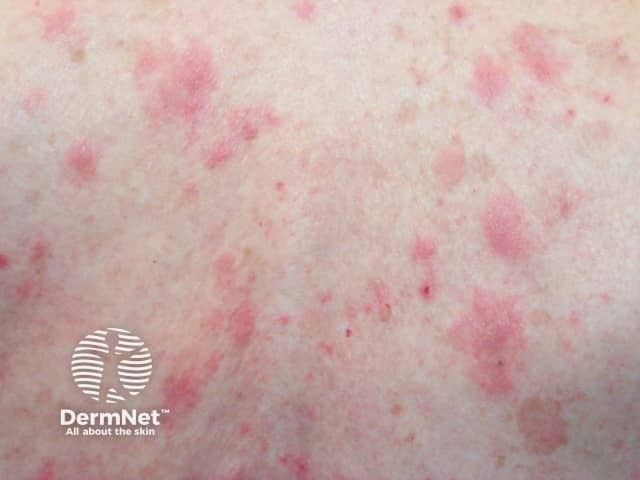
Bullous pemphigoid
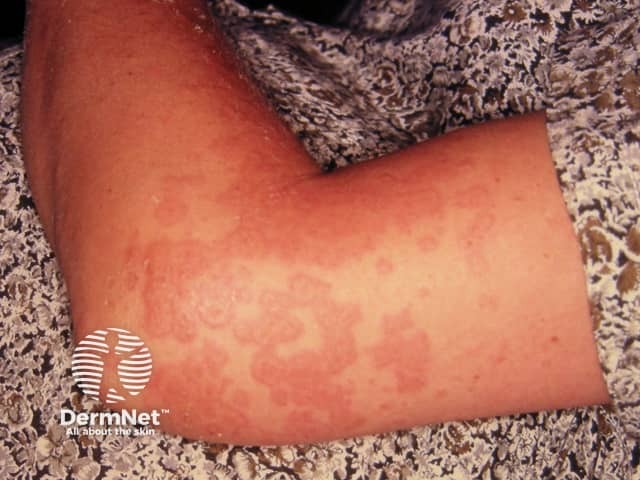
Pemphigoid gestationis
PUPPP or Pruritic Urticarial Papules and Plaques of Pregnancy is an eruption occurring during the last few weeks of pregnancy, usually in a first pregnancy.
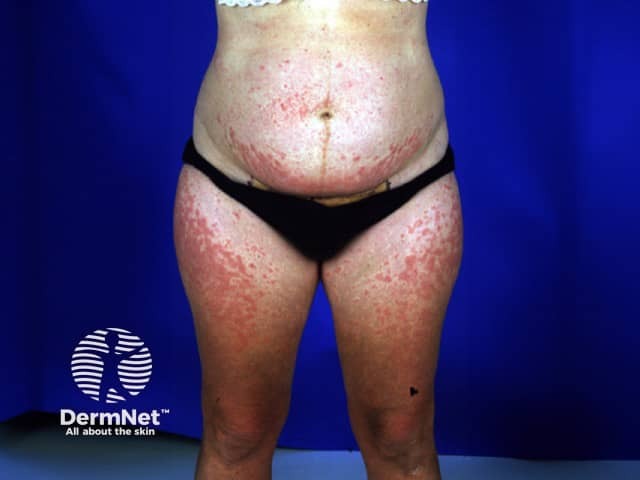
Polymorphic eruption of pregnancy PUPPP
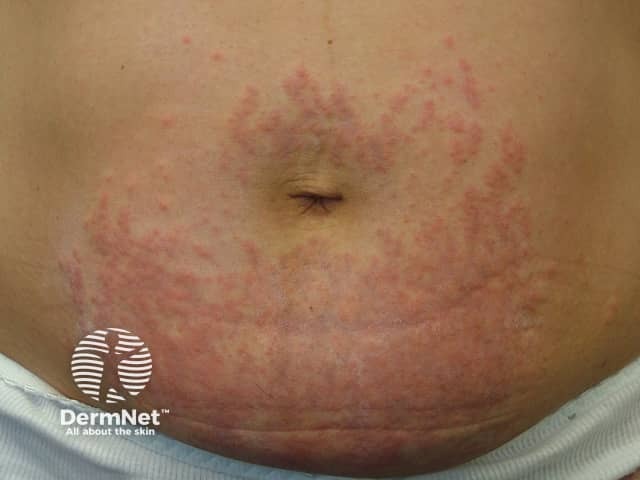
PUPPP polymorphous eruption of pregnancy
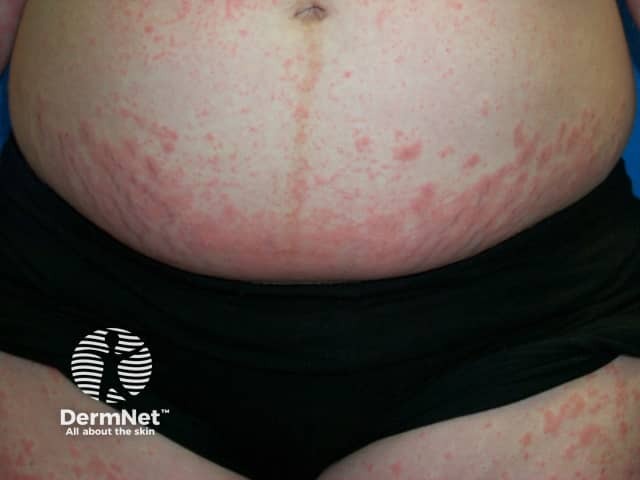
PUPPP polymorphous eruption of pregnancy
Annular erythema usually begins as a small raised pink-red spot that slowly enlarges and forms a ring shape while the central area flattens and clears. They may resemble an urticarial weal but often have a trailing scale. They are asymptomatic. The rings enlarge at a rate of about 2-5 mm/day until they reach a diameter of about 6-8 cm. Sometimes the lesions do not form complete rings but grow into irregular shapes.
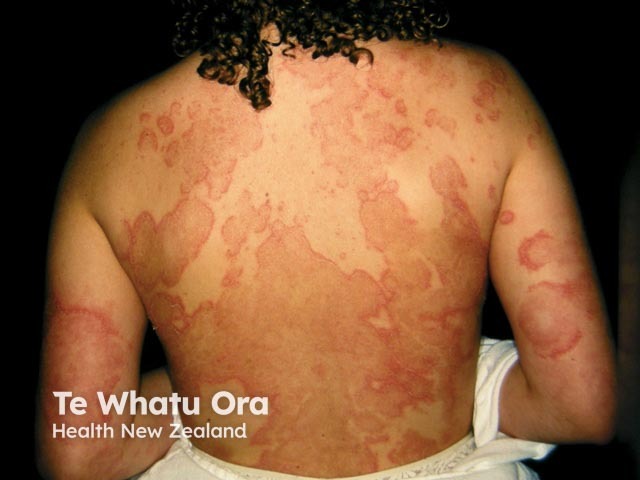
Annular erythema
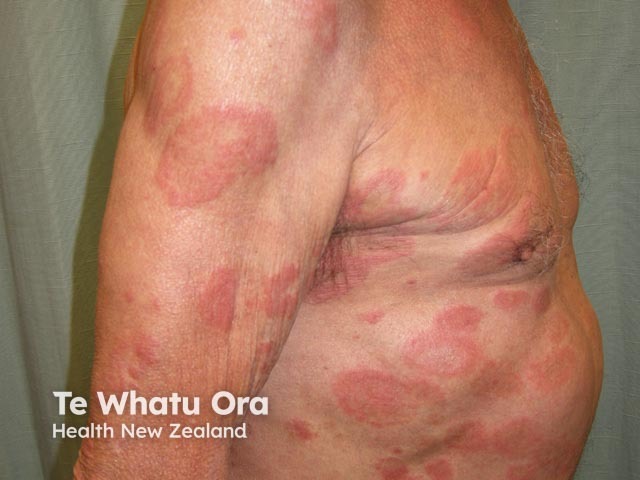
Annular erythema
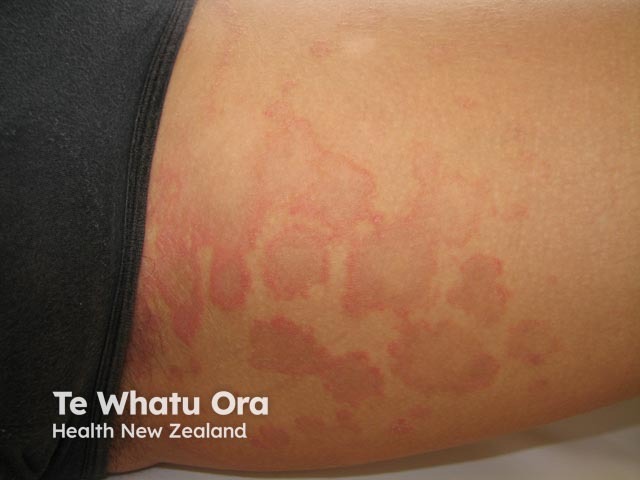
Annular erythema
Autoimmune progesterone dermatitis is a rare, recurrent and itchy rash affecting women during their childbearing years.
Interstitial granulomatous dermatitis is a distinctive pathological entity of an unusual persistent skin eruption often of an urticarial type. Other lesions described with the same pathology include papules, nodules and plaques that are skin coloured, red or brown. These may be oval, annular or cord-like.
Interstitial granulomatous dermatitis is associated with autoimmune diseases, particularly seronegative polyarthritis, and is occasionally seen in association with lymphoma, lung cancer, drugs and infections
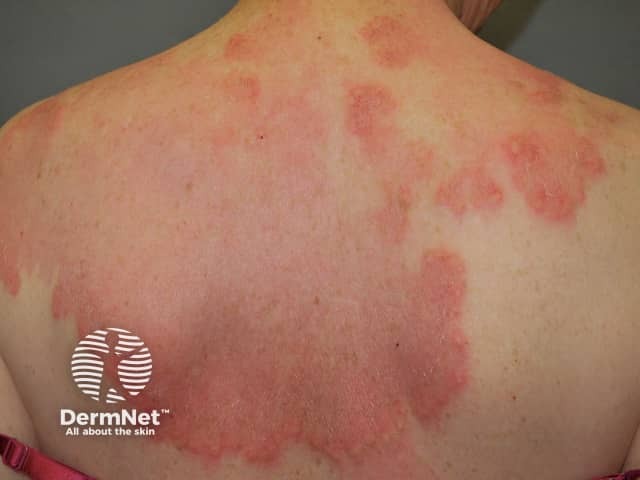
Interstitial granulomatous dermatitis
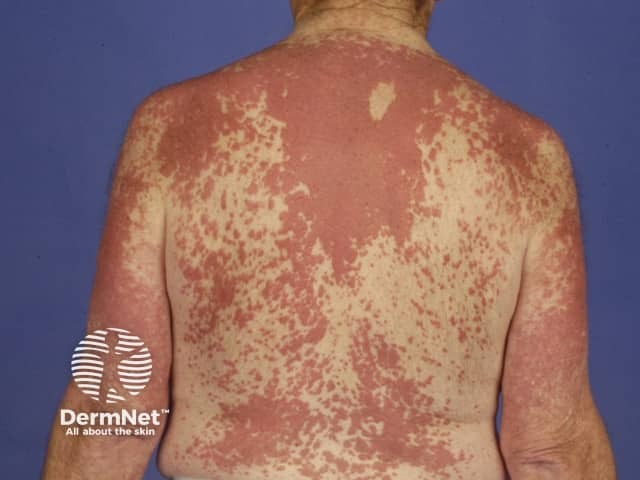
Interstitial granulomatous dermatitis
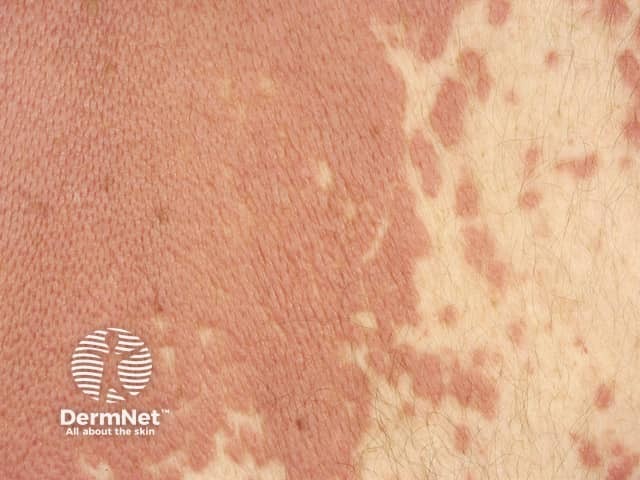
Interstitial granulomatous dermatitis
Wells syndrome, also called eosinophilic dermatitis, also presents with urticarial lesions. Eosinophils are seen in the blood in 50% of patients.
Skin biopsy is characterised by eosinophils and flame figures.
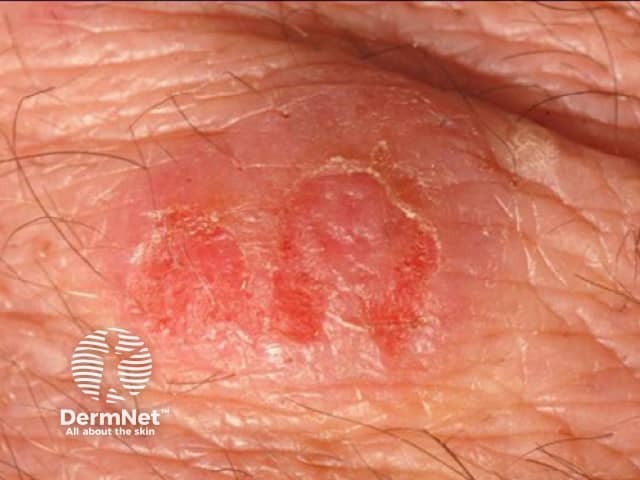
Wells syndrome
Neutrophilic eccrine hidradenitis is a rare condition occurring in patients with acute myelogenous leukaemia, either while on or after receiving chemotherapy.
Skin biopsy reveals neutrophils around the eccrine sweat glands and some destruction of eccrine cells.
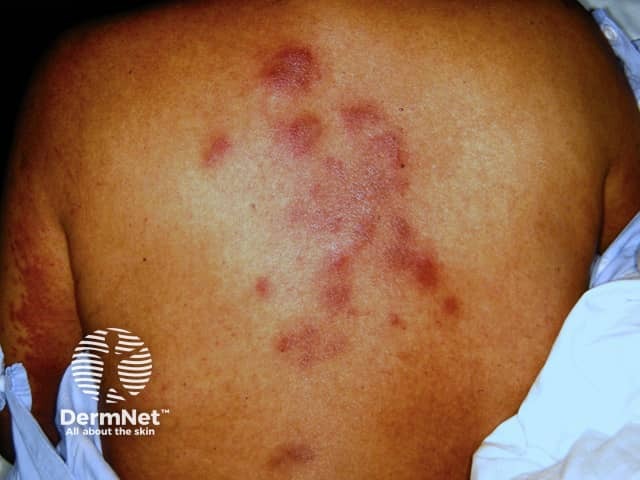
Neutrophilic eccrine hidradenitis
Patients with ordinary urticaria do not usually have systemic symptoms, so if these are present, other diagnoses should be considered.
Sudden onset of a red itchy rash within 30 minutes of consuming decomposing scombroid fish may be due to scombroid fish poisoning in which large amounts of histamine are ingested. Unlike urticaria, there are no weals. Other symptoms include a headache, palpitations, nausea, diarrhoea and collapse.
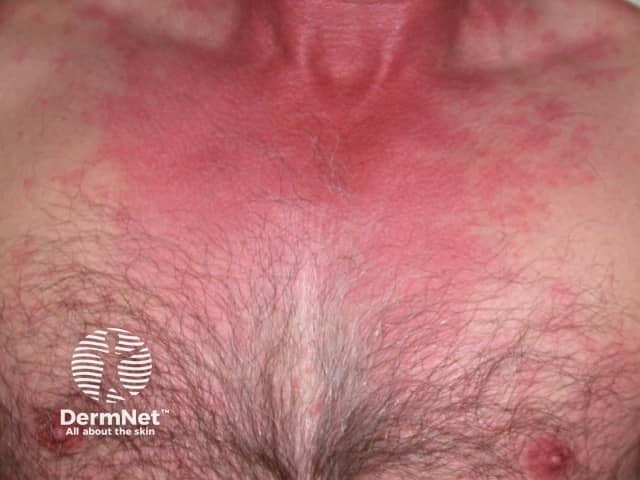
Scombroid rash
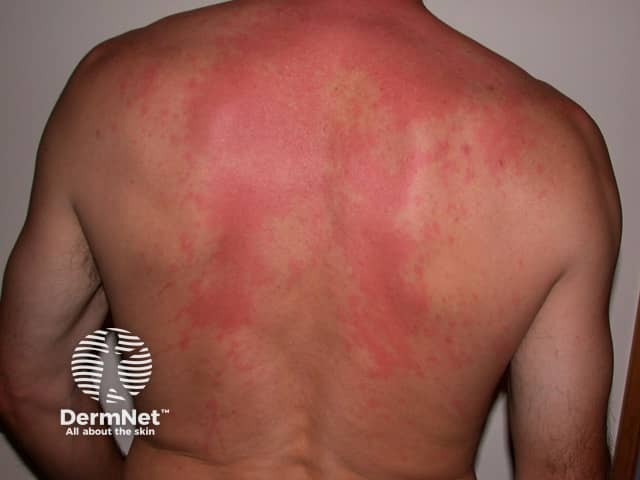
Scombroid rash
Urticarial vasculitis is defined by histology showing small vessel vasculitis on skin biopsy.
Hypersensitivity vasculitis, cutaneous polyarteritis nodosa and Churg-Strauss syndrome may also present with urticaria-like lesions.
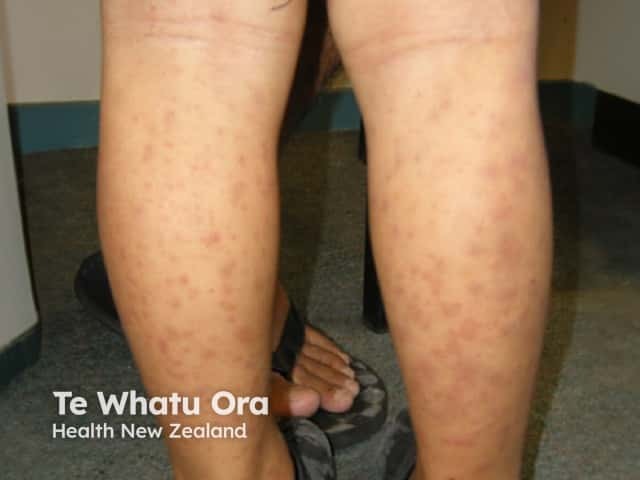
Urticarial vasculitis
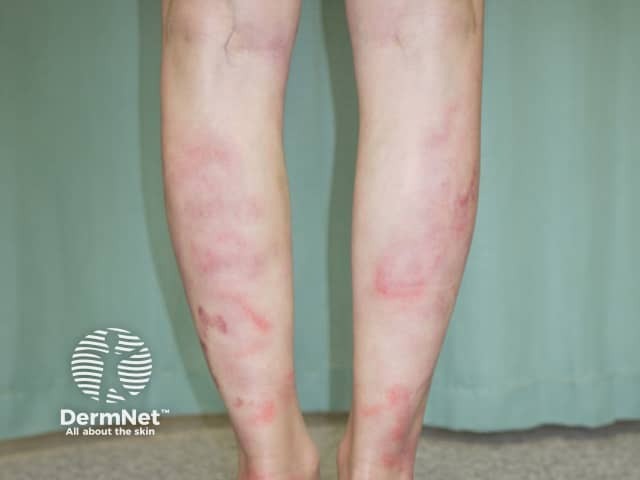
Urticarial vasculitis
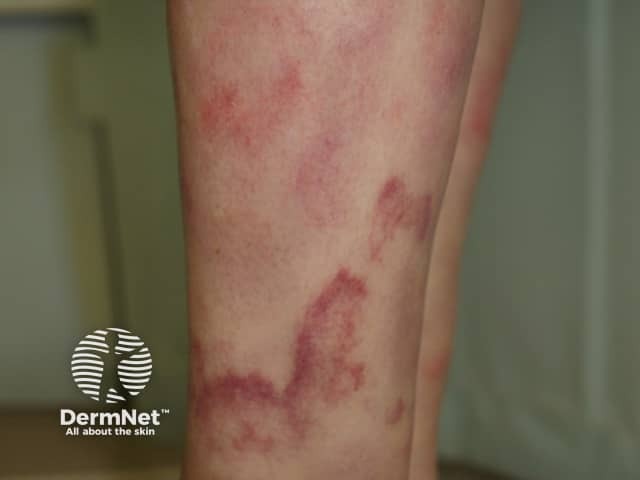
Urticarial vasculitis
Tender urticaria-like plaques may be seen in acute neutrophilic dermatosis (Sweet syndrome). The lesions often blister and may affect mucosal surfaces as well as skin surfaces. They are often seen on the neck but may occur on any site. The plaques enlarge and persist for days to weeks. Sweet syndrome results in fever, malaise, arthralgia, and other systemic symptoms.
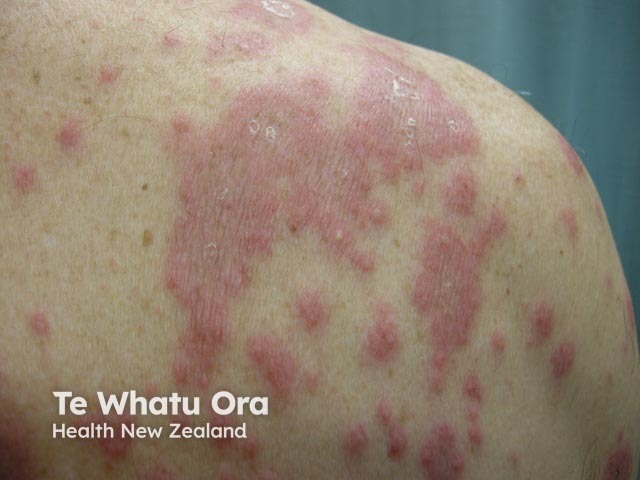
Sweet disease
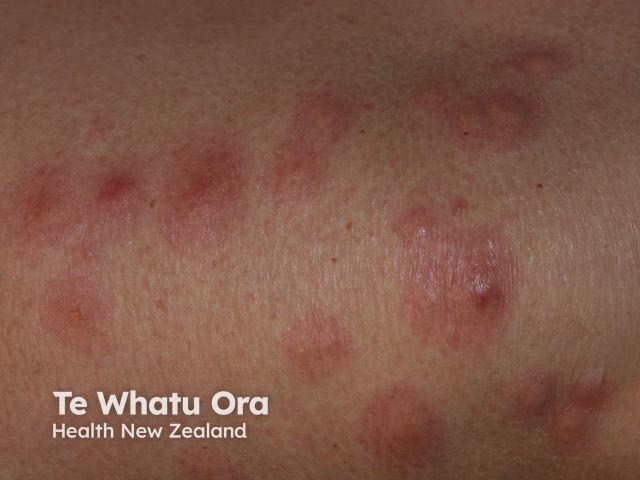
Sweet disease
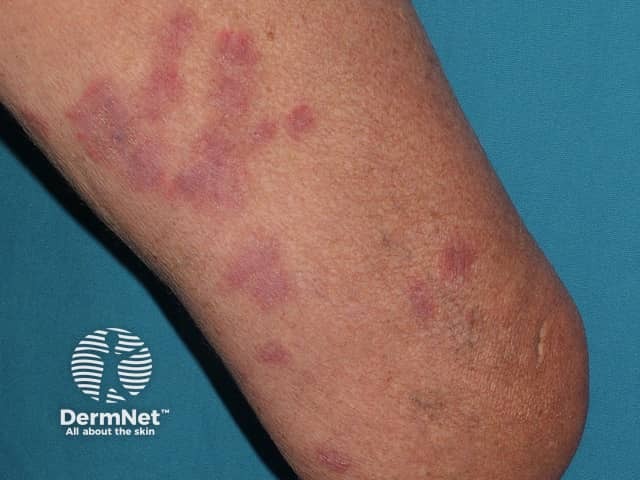
Sweet disease
Neutrophilic urticarial dermatosis presents with urticarial lesions that are defined by a histological reaction pattern revealing neutrophils lined up between collagen fibres.
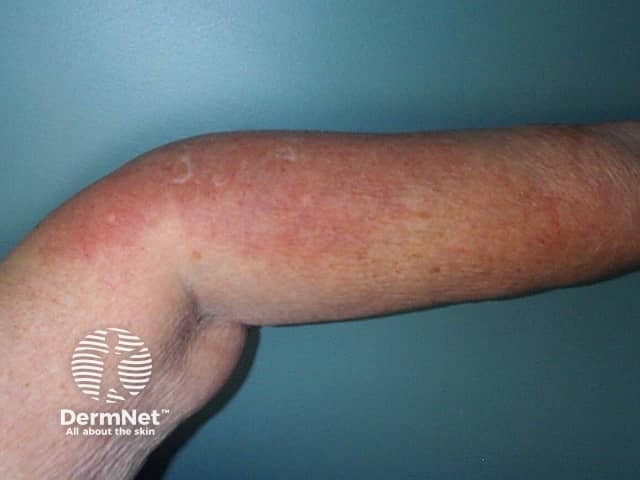
Neutrophilic dermatosis associated with rheumatoid arthritis
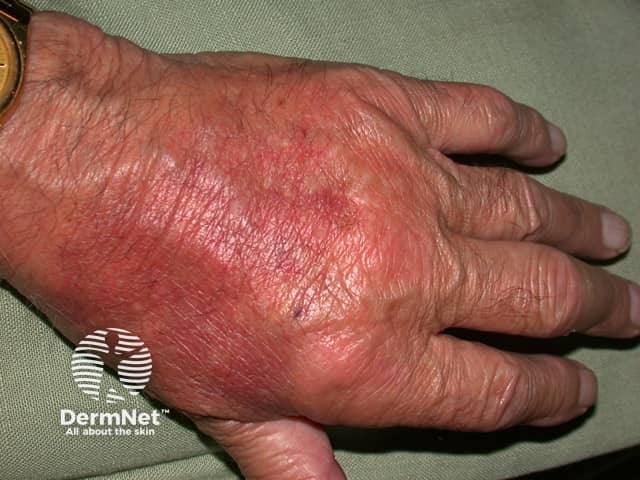
Neutrophilic dermatosis associated with rheumatoid arthritis
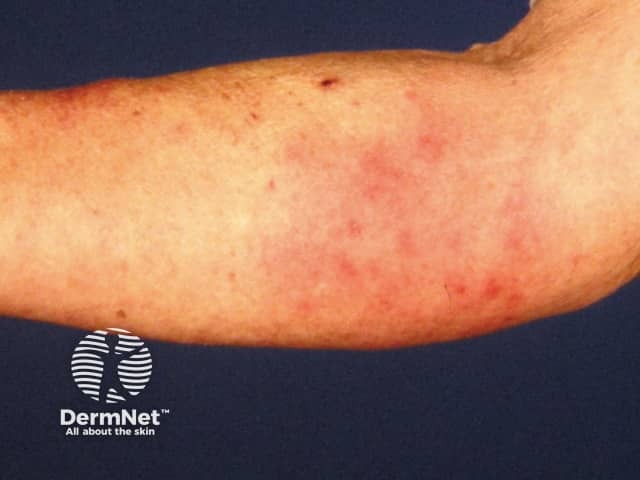
Neutrophilic dermatosis associated with rheumatoid arthritis
Eosinophilic dermatosis of haematological malignancy arises in some forms of leukaemia. The skin lesions may include urticarial plaques.
The autoinflammatory syndromes are a group of mainly genetic diseases that affect the skin and other organs.
An urticated erythema means a rash with raised red patches. This includes many of the conditions described above. When accompanying upper respiratory symptoms, such as a sore throat, fever and malaise, it is often due to the underlying viral infection and is a type of exanthem. An exanthem with flat red patches may also be called toxic erythema.