Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Joel Winders, medical student, University of Auckland, Department of Dermatology, Waikato Hospital, Hamilton, New Zealand. DermNet New Zealand Editor in Chief: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy editors: Gus Mitchell/Maria McGivern. October 2017.
Introduction - granuloma
Introduction - foreign body
Introduction - foreign body granuloma
Immune response
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
A granuloma is a histological term for a collection of histiocytes or epithelioid histiocytes accompanied by a range of multinucleated giant cells (masses of macrophages) and other inflammatory cells [1].
A foreign body is any material, living or non–living, that is recognised by host immunity to be 'non-self' and elicits an immunological response.
A foreign body granuloma forms in response to the introduction of exogenous material to the skin, or in response to modified endogenous material that the immune system identifies as foreign [3].
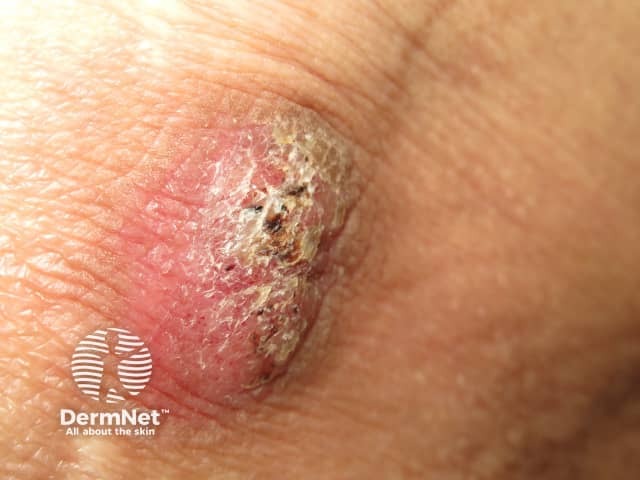
Silica granuloma
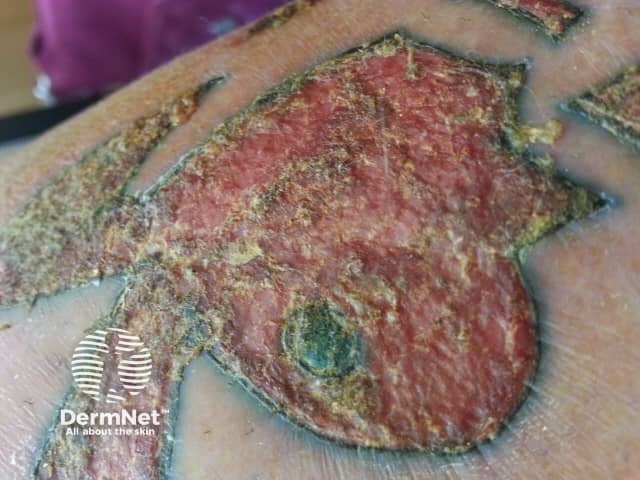
Tattoo granuloma
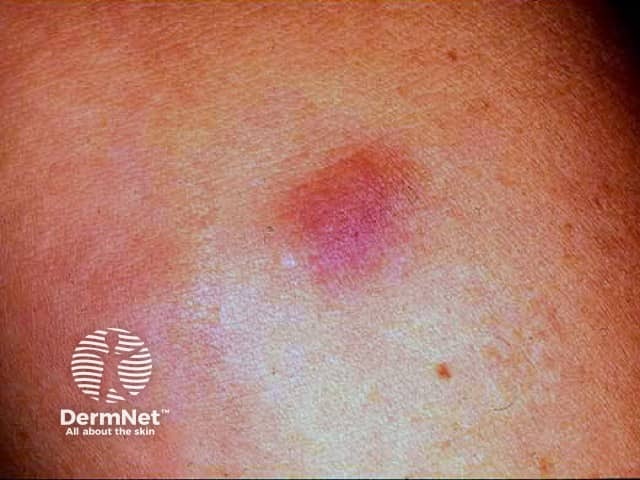
Bovine collagen granuloma
The body mounts an inflammatory reaction to get rid of foreign bodies. Neutrophils form the initial host defence by attempting to envelop and digest (phagocytose) the foreign material. If this response is not sufficient in eliminating the foreign body, then monocytes and local tissue macrophages will be activated to engulf the foreign material. If the foreign body is small enough, these cells will effectively remove it from the tissue [1–3].
If foreign bodies are present on the surface of the skin (such as debris in a wound), keratinocytes migrate along the connective tissue formed by fibrin, fibronectin and type V collagen, and dissect it from the underlying tissue during the proliferative phase of healing.
Foreign bodies are most commonly introduced into the body through voluntary means, such as tattoos and cosmetic fillers. Involuntary causes of foreign body granulomas, such as minerals and metals accidentally imbedded in the skin, are often seen in those who work in construction industries [3].
A foreign body granuloma forms when the host immune system is unable to digest the foreign body, resulting in the accumulation of macrophages and histiocytes. As macrophages surround and isolate the foreign body, some of them will fuse to form multinucleated giant cells. T cells and fibroblasts also participate in this inflammatory response [3].
Substances that cause foreign body granulomas include:
Foreign body granulomas most commonly appear as red or red-brown papules, nodules or plaques, which may or may not ulcerate [2,3].
Tattoo granulomas are normally confined to the area of the tattoo. They are most often tender erythematous nodules. Lichenoid or eczematous plaques may also occur. Granulomas usually arise after a new tattoo, although delayed reactions have been reported up to 17 years after tattoo placement.
Hypersensitivity reactions to bovine collagen result in induration and erythema in the area where the collagen has been injected. Sterile abscesses may occur, which can last for several months or longer.
Silicone granulomas can form in the dermis when trauma causes the capsule around a silicone implant to rupture. Larger nodules, ulcers and sclerosis may slowly develop, months to years after the injury. Distant nodules can also form due to the leakage of silicone into dependent sites.
Subcutaneous liquid silicone injections may also result in cutaneous nodules and indurated or ulcerated plaques.
Paraffin injection for breast or penile implants can lead to a firm, non-tender, nodule, an indurated and ulcerated plaque, and an abscess at the site of injection. This reaction is known as sclerosing lipogranuloma or oleogranuloma.
A nodule may form at the site of intralesional corticosteroid injection, due to incomplete absorption or unusual dispersion of the injected material.
Papules, nodules and indurated plaques may develop within a scar after trauma involving glass, sand and dirt.
Aluminium can be introduced into the body through vaccines and immunotherapy. Granulomas may appear as persistent subcutaneous nodules some months after injection.
Granulomas are a rare side effect of insulin injections containing zinc. They present as sterile furuncles (boils), which later heal with atrophic scarring at the injection site.
Talc (hydrous magnesium silicate) is found in many antibiotic and dusting powders and may cause granulomas if these powders are applied to open wounds. Talc granulomas are erythematous papules or nodules that can take years to appear. Reported sites include the umbilicus of infants, amputation stumps, injection sites and the inguinal area.
The retained suture material can be responsible for an inflamed wound site a few weeks after a cutaneous surgical procedure. A fistula to the skin surface may form, and the suture may be ejected from the skin (spitting sutures). Natural materials, such as gut, are more likely to 'spit' than monofilament nylon.
Cactus spines can induce an acute inflammatory reaction and produce clusters of skin-coloured dome-shaped papules, each with a black dot in the centre. These are found on the hands and fingers of people who handle cactus fruit. A similar reaction can affect people handling sea urchins.
Complications of foreign body granuloma can include:
Clinical history and examination are often adequate to diagnose foreign body granuloma. Investigations may include:
The differential diagnosis of foreign body granulomas includes other forms of granuloma and other reactions to foreign bodies (for example in-growing hairs can cause pseudofolliculitis, especially in the beard area). The differential diagnoses include:
Foreign body granulomas can be excised. Other methods of removal depend on the cause.
The gold standard for the removal of superficial skin tattoos is non-ablative quality (Q)-switched lasers. Picosecond lasers have also been used. The surgical removal of deeper tattoo granulomas may be required.
Topical steroids, intralesional steroid injections, tacrolimus, imiquimod and etanercept have been used successfully to treat granulomatous tattoo reactions.
Foreign body granulomas due to cosmetic fillers may be treated with antibiotics, oral steroids, and intralesional corticosteroid injections. Fluorouracil injections have also been used. Surgical removal may be undertaken if other treatment options fail.
Other medical options used to treat foreign body granulomas include:
The natural history of foreign body granuloma varies depending on the cause. Foreign body granulomas and abscesses due to bovine collagen injections often regress spontaneously within 1–2 years [2–4]. Other types of foreign body granuloma may persist for decades.
Skin-nontumor: Foreign body reaction — PathologyOutlines.com