Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Bob Chan, Dermatology Registrar, Auckland, New Zealand, November 2014.
Mid-dermal elastolysis is a rare, acquired skin condition of elastic tissues. Elastic fibres provide skin tissue with elastic recoil and resilience. In mid-dermal elastolysis, there is a selective loss of elastic fibres in the mid-dermis.
Mid-dermal elastolysis has been reported mostly in Caucasian patients, with a female predominance. The most commonly affected sites are the trunk and upper arms; the face and lower legs are only occasionally affected.
There have been 3 clinical subtypes of mid-dermal elastolysis described.
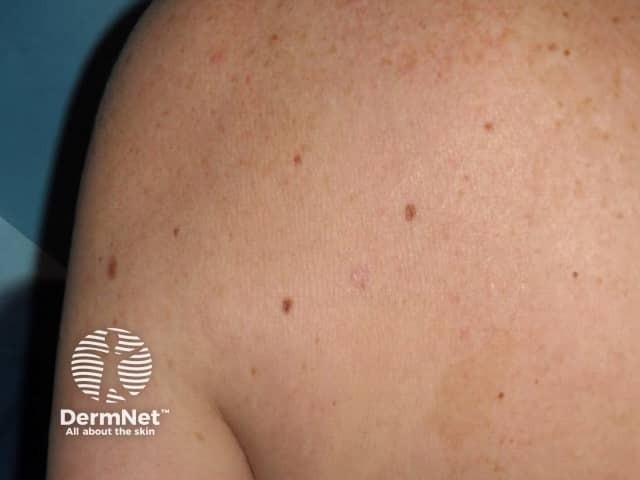
Mid-dermal elastolysis
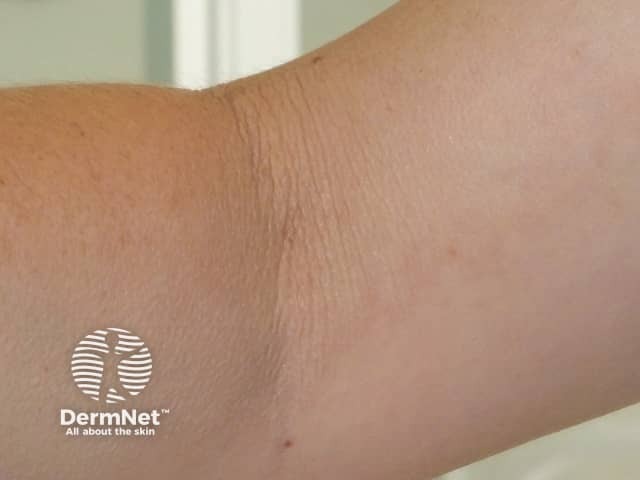
Mid-dermal elastolysis
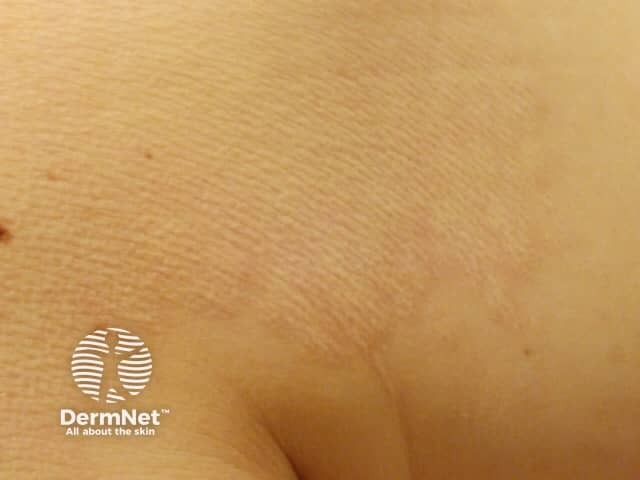
Mid-dermal elastolysis
The exact cause of mid-dermal elastolysis is unknown. It is associated with localised increased activity of elastase, an enzyme involved in elastin breakdown.
Reported associations with mid-dermal elastolysis include:
Biopsy features can be helpful to confirm the diagnosis of mid-dermal elastolysis. Specimens may appear normal with haematoxylin and eosin stain (H&E) or may have a discrete inflammatory infiltrate. Band-like or focal loss of elastic fibres can be seen in the mid-dermis with elastic stains.
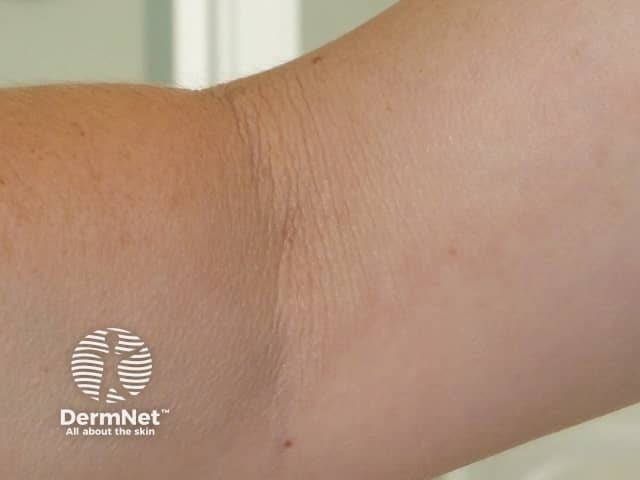
Mid-dermal elastolysis
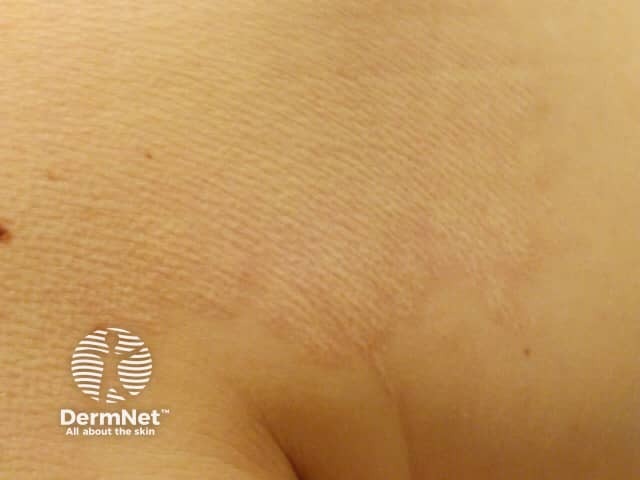
Mid-dermal elastolysis
Sun protection is recommended as UV radiation is a possible cause of mid-dermal elastolysis. Topical retinoids may improve the appearance of wrinkling.
Other treatments, including topical and systemic steroids, hydroxychloroquine, vitamin E, clofazimine, and colchicine have not been shown to be beneficial.