Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Delwyn Dyall-Smith FACD, Dermatologist, 2010. Minor update November 2025.
Introduction
Demographics
Clinical features
Diagnosis
Treatment
Orofacial granulomatosis (as defined by Wiesenfeld in 1985) is the specific histology finding of granulomas in mucosal or skin biopsies taken from the mouth or face in the absence of a recognised systemic condition known to cause granulomas. It, therefore, includes Melkersson-Rosenthal syndrome and Miescher cheilitis (granulomatous cheilitis) but excludes Crohn disease, sarcoidosis and granulomatosis with polyangiitis.
Note that the term orofacial granulomatosis is often used loosely to mean any diagnosis of granulomas in the orofacial region, including orofacial Crohn disease and sarcoidosis, and may also be used to describe patients with a similar presentation in whom granulomas have not been found on biopsy.
In this summary, the strict definition of idiopathic disease is followed.
Orofacial granulomatosis is an uncommon condition that has been reported in nearly all age groups and races. It affects males and females equally. Although the literature suggests it is more common in younger age groups, this may include patients with Crohn disease as most children diagnosed with granulomas in orofacial sites are subsequently found to have Crohn disease.
The cause of orofacial granulomatosis is unknown. However, it may represent an abnormal immune response in someone with predisposing genetic factors. Unrecognised food allergies (eg, to benzoic acid, flavourings, cinnamaldehyde, cinnamon, and chocolate in food), reactions to dental materials, and infections have all been proposed, although the evidence for these is not strong. Sodium metabisulphite contact allergy (common food/drink preservative) was attributed in a single case; the condition resolved on allergen avoidance.
It is believed the granulomas block the lymphatic vessels resulting in lymphoedema.
The most common clinical presentation is painless swelling of one or both lips. Involvement of the lower lip is the most common. Initially, the swelling is soft and comes and goes, with each episode lasting weeks or months. Eventually, the lip enlargement becomes permanent and the lip feels firm or rubbery. This is clinically indistinguishable from orofacial Crohn disease and sarcoidosis.
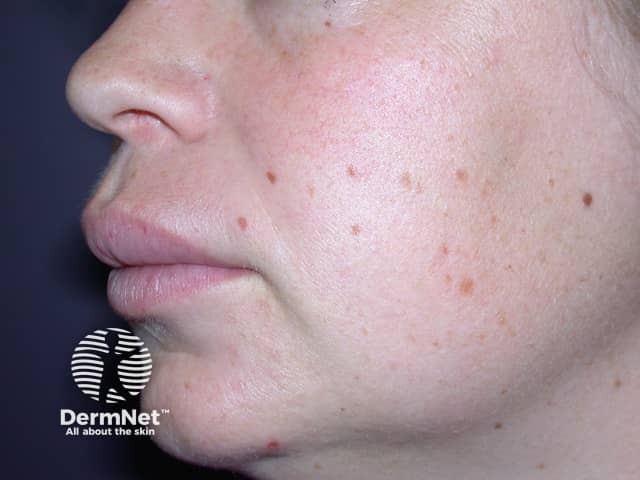
If the lips become very protuberant, fissuring (cracking) may occur in the midline of the lips (median cheilitis) or at the angles of the mouth (angular cheilitis). A lip-licking habit may result in irritant contact dermatitis. The skin around the mouth may become dry, red and peeling.
The lip swelling may become severe enough to interfere with speech and eating.
Swelling may also occur inside the mouth, affecting the inside of the cheeks or lips to produce a cobblestoned appearance, or causing enlargement of the gums or tongue.
A similar pattern of swelling may affect other regions of the face such as around the eyes, cheeks, or chin.
Other signs in the mouth of orofacial granulomatosis may include:
Facial nerve paralysis may also be associated with orofacial granulomatosis as in Melkersson-Rosenthal syndrome.
Granulomatous cheilitis
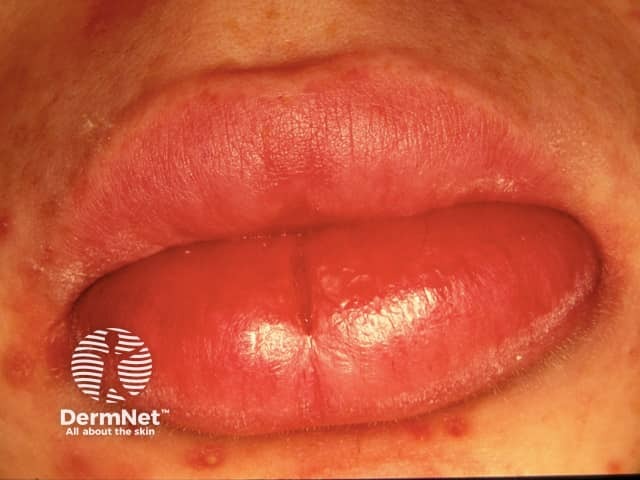
Granulomatous cheilitis
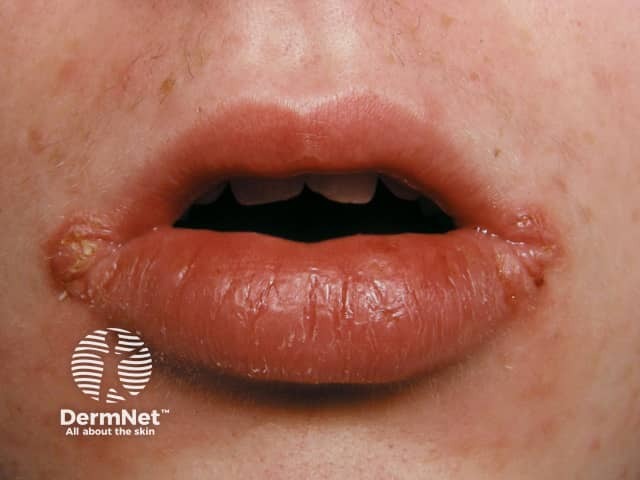
Granulomatous cheilitis
The diagnosis of orofacial granulomatosis is based on the clinical history of recurrent oral or facial swelling that becomes permanent and the presence of noncaseating granulomas on deep incisional biopsy. However, granulomas are seen in less than 50% of cases. Dilated lymphatics and blood vessels, oedema and nonspecific inflammation are commonly seen. Special stains for infections and polarised light microscopy for foreign material should be negative.
Recognised causes of granulomas such as tuberculosis, sarcoidosis and Crohn disease must be excluded. Further investigations may include:
These should all be normal/negative in orofacial granulomatosis. The role of allergy testing is not clear.
There are reports of Crohn disease developing years after the orofacial symptoms, so reassessment may be required, particularly if new symptoms develop such as abdominal pain or diarrhoea.
As the cause of orofacial granulomatosis has not been determined, there is no curative treatment. Spontaneous remission can occur but is rare. Treatment is offered where there is pain, cosmetic concerns or impaired function.
Corticosteroids are the most commonly used treatments:
Oral tetracycline, anaerobic antibiotics such as metronidazole, or dapsone are sometimes helpful in reducing swelling.
Topical tacrolimus alone or in combination with other treatments has also been used for mild swelling.
Another immunomodulating treatment is often required in addition to the steroid. Methotrexate, hydroxychloroquine, clofazimine, azathioprine and low dose thalidomide have been reported to help in small case series. Anti-TNFα inhibitors such as infliximab have also been used successfully.
Response to treatment is slow. Partial or complete improvement can be observed in most but not all patients, although this can take years. Swelling is more likely to improve than oral ulceration.
Surgery may be required for severe permanent swelling interfering with speaking or eating.