What is psoriatic arthritis?
Psoriatic arthritis is a painful, inflammatory condition of the joints that can occur in up to 30 per cent of patients with psoriasis.
Who gets psoriatic arthritis?
Psoriatic arthritis has an incidence of approximately 6 per 100,000 per year and a prevalence of about 1–2 per 1000 in the general population. Estimates of the prevalence of psoriatic arthritis among patients with psoriasis range between 4 and 30 per cent. In most patients, arthritis appears 10 years after the first signs of skin psoriasis. The first signs of psoriatic arthritis usually occur between the ages of 30 and 50 years of age. In approximately 13–17% of cases, arthritis precedes the skin disease.
Men and women are equally affected. The symptoms of psoriatic arthritis come and go but it is a lifelong condition that is usually progressive.
Patients with psoriasis who are more likely to subsequently get arthritis include those with the following characteristics:
- Psoriatic nail disease
- Flexural psoriasis, scalp psoriasis or post-auricular psoriasis
- Obesity
- Smoker
- Elevated C-reactive protein (CRP) at baseline.
Classification of psoriatic arthritis
Psoriatic arthritis is a form of spondyloarthritis. Spondyloarthritis is an umbrella term used to describe a family of disorders, including ankylosing spondylitis, non-radiographic axial spondyloarthritis, psoriatic arthritis, reactive arthritis, enteropathic arthritis and undifferentiated spondyloarthritis. These different forms of spondyloarthritis share several clinical features:
- Axial joint inflammation (especially the sacroiliac joints)
- Asymmetric oligoarthritis (especially of the lower extremities)
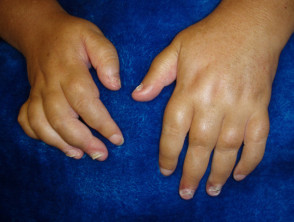
- Dactylitis: 'sausage digits' (very swollen fingers or toes that look like sausages)
- Enthesitis: pain and swelling at the insertion of tendons and ligaments, commonly at the heel, tibial tuberosity and humerus; this affects up to 53% of patients with psoriatic arthritis
- Negative Rheumatoid Factor
- HLA-B27 positivity: HLA-B27 is a specific protein involved with immune regulation. 57% of psoriatic arthritis patients with axial involvement are positive for HLA-B27
- Genetic susceptibility to the condition/family history
- Distinctive radiological features.
What causes psoriatic arthritis?
The main contributing factors to the development of psoriatic arthritis are a genetic predisposition, immune factors and the environment.
Genetic predisposition
As in psoriasis of the skin, many patients with psoriatic arthritis may have a familial tendency toward the condition. A twin study found that arthritis was as common in dizygotic (fraternal) twins as in monozygotic (identical) twins so unknown environmental factors may also be important. First-degree relatives of patients with psoriatic arthritis have a 50-fold increased risk of developing psoriatic arthritis compared with the general population. It is unclear whether this is due to a genetic basis of psoriasis alone, or whether there is a special genetic predisposition to arthritis as well.
Immune factors
Psoriatic arthritis occurs as a result of abnormal interaction between the immune system and the joints. People with psoriatic arthritis seem to have an overactive immune system as evidenced by raised inflammatory markers, increased antibodies and T-lymphocytes.
Activated T cells (in particular CD8+ T cells) have generally been found in the skin and joints of patients with psoriatic arthritis. Several studies have demonstrated that pro-inflammatory cytokines secreted from activated T cells (especially tumour necrosis factor alpha (TNF-α), IL-17, IL-18 and IL-23) induce proliferation and activation of synovial and epidermal fibroblasts. CD8+, IL-17+ cells, natural killer (NK) cells and innate lymphoid (ILC3) cells are present in high concentrations in the synovial fluid and skin lesions in patients with psoriatic arthritis.
The environment
Environmental factors implicated in the pathogenesis of psoriatic arthritis include infections (bacterial infections such as streptococci and Borrelia burgdorferi, the cause of Lyme disease; and viral infections such as rubella), trauma (Koebner phenomenon), moving to a new house, recurrent oral ulcers, obesity and bone fractures.
An inverse association with smoking has also been reported in HLA-C*06 allele negative patients.
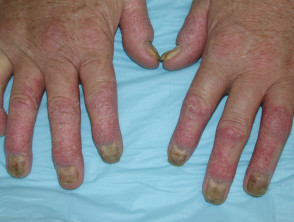
What are the signs and symptoms of psoriatic arthritis?
Psoriatic arthritis
Joint manifestations
There are 5 main patterns of joint involvement:
- Distal arthritis
- Asymmetric oligoarthritis (60%)
- Symmetric polyarthritis
- Spondyloarthritis (axial involvement)
- Arthritis mutilans (5%).
Large and small joints may be affected.
- Distal interphalangeal involvement is a hallmark of psoriatic arthritis and can be difficult to distinguish from osteoarthritis.
- Symptoms include joint pain, swelling and stiffness.
- Specific problems include difficulties with using the hands, standing for long periods and walking.
- Psoriatic arthritis may result in severe damage to the joints and can be as severe as rheumatoid arthritis.
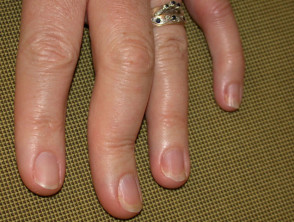
Psoriatic nail disease
Nail lesions occur in 90% of patients with psoriatic arthritis. The severity of psoriatic nail involvement may correlate with the extent and severity of both skin and joint disease. Psoriatic nail dystrophy can be difficult to distinguish from fungal nail infection. Characteristic features include:
- Nail pits: defined depressions in the plate caused by shedding of nail plate cells
- Onycholysis: separation of the nail from its bed
- Distal nail bed hyperkeratosis
- Splinter haemorrhages.
Other features of psoriatic arthritis
- Enthesitis
- Dactylitis
- Fatigue
- Mouth ulcers
Co-morbidities associated with psoriatic arthritis include:
- Ocular involvement: uveitis (7%) and conjunctivitis (20%).
- Cardiovascular disease
- Inflammatory bowel disease
- Metabolic syndrome
- Hypertension
- Diabetes
- Atherosclerosis
- Depression and anxiety.
What is the association with psoriasis of the skin?
People with psoriatic arthritis usually have some skin signs eventually.
Psoriatic arthritis develops after skin psoriasis in approximately 75% of patients. Remaining patients have either a simultaneous onset of skin and joint psoriasis (10%), or joint symptoms precede any skin problem (15%). The severity of the skin disease does not predict the severity of the joint disease.
Plaque psoriasis is the most common form of skin psoriasis seen with psoriatic arthritis. Joint symptoms may be exacerbated by a flare in skin psoriasis but quite commonly the skin symptoms behave independently of joint symptoms. Most people with psoriatic arthritis have mild psoriasis.
How is psoriatic arthritis diagnosed?
The diagnosis of psoriatic arthritis is based on symptoms, an examination of skin and joints and compatible X-ray findings. The diagnosis of psoriatic arthritis may be difficult due to its varied clinical presentation. Psoriatic arthritis may present with tendinitis, enthesitis or dactylitis, rather than swollen joints.
X-ray findings that are characteristic of psoriatic arthritis include:
- Changes affecting the joints at the end of the fingers and toes
- Asymmetrical joint involvement (particularly of the sacroiliac joints)
- Erosions: Destruction of the bone and cartilage adjacent to joint spaces
- “Pencil-in-cup” deformity: results from periarticular erosions and bone resorption giving the appearance of a pencil in a cup.
- Subluxation: slipping of the alignment of the joint
- Ankylosis: fusion of bones together across the joint space
- Wispy and dense bony outgrowths around joints ('whiskering' and 'spurs', respectively)
- Increased calcium salt deposition around the insertion of ligaments and tendons into the bone and other features of enthesopathy.
- Ivory phalanx: increased radiodensity of an entire phalanx as a result of periosteal and endosteal bone formation.
X-rays in psoriatic arthritis
Other conditions with similar clinical and X-ray findings to psoriatic arthritis include:
- Rheumatoid arthritis
- Gout
- Osteoarthritis
- Reactive arthritis
- Ankylosing spondylitis.
MRI and ultrasound can also aid diagnosis, by identifying enthesitis, tendinitis and ligamentous inflammation.
There are no diagnostic blood tests for psoriatic arthritis but tests may be done to help confirm the diagnosis and rule out other causes.
- Markers of inflammation, ESR (erythrocyte sedimentation rate) and CRP, may reflect the severity of the inflammation in the joints.
- Rheumatoid factor is usually negative but may be positive in up to 10% of patients with psoriatic arthritis.
- Anti-CCP (anti-cyclic citrullinated peptide) is also usually negative but may be positive in up to 7% of patients with psoriatic arthritis.
- HLA-B27 testing
Classification criteria, such as CASPAR criteria, are mainly used for research purposes. Several screening questionnaires have also been developed, such as Toronto Psoriatic Arthritis Screen (ToPAS2), to help to identify patients with psoriatic arthritis.
What treatment is available for psoriatic arthritis?
Some treatments for joint psoriasis are also effective for skin psoriasis, so treatment plans may take both skin and joint disease into account.
The principles of treatment include early and aggressive treatment in order to prevent joint deformity and resulting morbidity. The choice of treatment depends on disease manifestation (pattern of joint involvement, the severity of joint vs skin involvement, non-articular involvement) in addition to factors regarding safety (regarding comorbidities), tolerability and patient preference.
Non-pharmacological management strategies are important; these include physical and occupational therapy, exercise, prescription of orthotics, and education regarding the disease and about joint protection, disease management, and the proper use of medications. Patients should receive assistance in weight reduction and management of cardiovascular risk factors and other comorbidities
In general, a stepwise approach to pharmacological treatment is adopted:
Step one
If arthritis is mild and limited to a few joints and the skin disease is not severe, the skin is treated with topical therapies or phototherapy and the joint disease is managed with pain relief (non-steroidal anti-inflammatory drugs, heat and ice) and possibly corticosteroid injections into the joint.
Step two
Non-biological disease-modifying antirheumatic drugs (DMARDs) improve symptoms of pain and stiffness, but none have been shown to prevent progressive joint damage and all have the potential for serious side effects. The following medications have a beneficial effect on joint disease and psoriasis:
Systemic steroids may help arthritis but can often cause a flare of psoriasis on reduction in dose or discontinuation.
Step three
Biological DMARDs: TNF-alpha inhibitors
Biologic response modifiers licensed for use in psoriatic arthritis are:
- Adalimumab
- Etanercept
- Infliximab
- Golimumab.
Step four
Other agents that are under investigation or are available include:
- Abatacept: (CTLA4-Ig) a selective T-cell co-stimulation modulator
- Tofacitinib: a Janus kinase (JAK1 and 3) inhibitor
- Secukinumab, brodalumab, ixekizumab: anti-IL-17 therapies
- Ustekinumab: a human monoclonal antibody to the shared p40 subunit of IL-13 and IL-23
- Filgotinib: a JAK1 inhibitor
- Guselkumab: an anti-leukin (IL)-23 monoclonal antibody
- Upadacitinib: JAK inhibitor.
Step five
In some cases, the joint disease may require orthopaedic surgery.
What is the long-term prognosis for psoriatic arthritis?
Most people with psoriatic arthritis will have ongoing problems with arthritis throughout the rest of their life. Remissions are uncommon; occurring in less than 20% of patients with less than 10% of patients having a complete remission off all medication with no signs of joint damage on X-rays. People with severe psoriatic arthritis have been reported to have a shorter lifespan than average.
Features associated with a relatively good prognosis are:
- Male sex
- Fewer joints involved
- Good functional status at presentation
- Previous remission in symptoms.
Features associated with a poor prognosis include:
- ESR > 15 mm/hr or raised CRP at presentation
- Failure of previous medication trials
- Absence of nail changes
- Joint damage (clinically or radiographically)
- HLA-B27-, -B39-, or -DQw3-positive status.