Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Kate Dear, Senior House Officer, St Mary’s Hospital, London, United Kingdom. DermNet New Zealand Editor in Chief: A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell, November 2017.
A respiratory disease refers to any condition that affects the upper respiratory tract, trachea, lungs, and the nerves and muscles associated with breathing. The correct recognition of cutaneous signs of respiratory disease can aid clinicians in diagnosing and treating these potentially life-threatening diseases.
Cyanosis is a blue discolouration of the skin and mucous membranes. It is seen in patients with more than 5 g/dL of desaturated haemoglobin. Cyanosis may be:
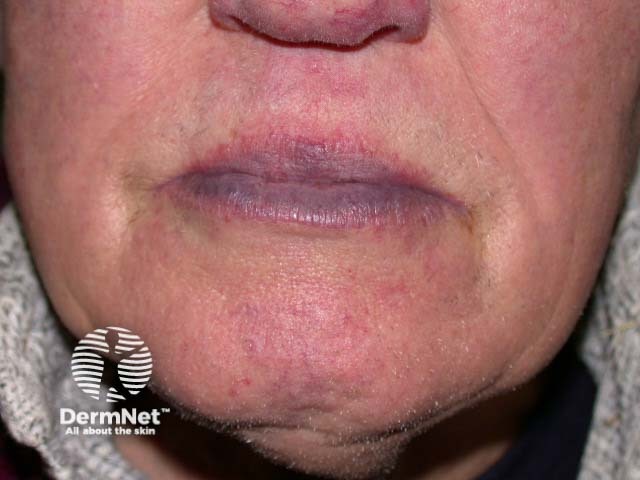
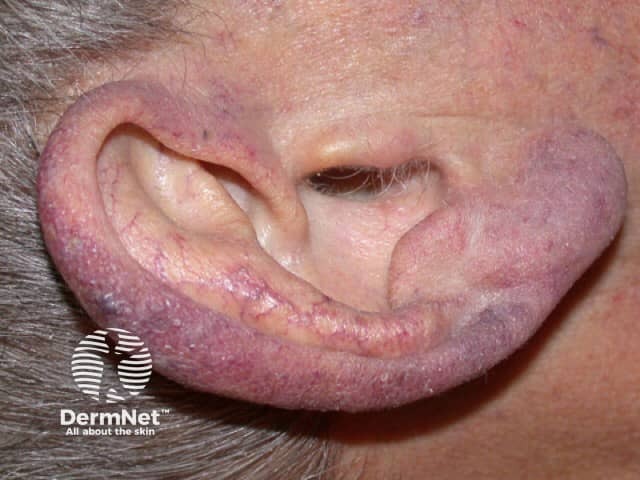
Cyanosis
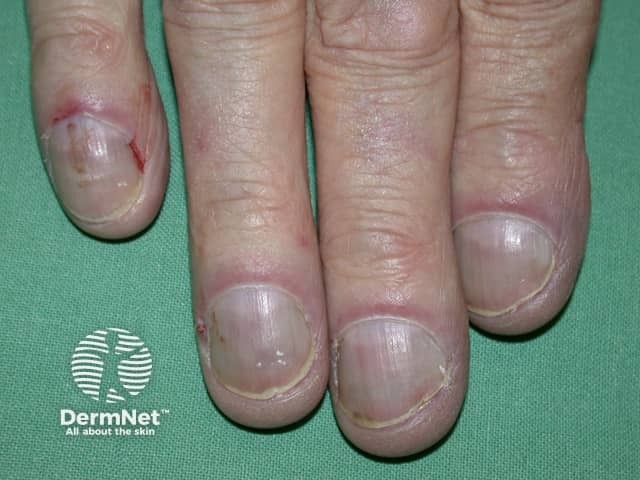
Cyanosis and clubbing
Nail clubbing is a deformity of the nails characterised by:
Clubbing is associated with a wide range of diseases, including the following respiratory diseases:
Hypertrophic osteoarthropathy comprises:
Symptoms of hypertrophic osteoarthropathy may precede the diagnosis of lung cancer and are most commonly associated with non-small-cell lung cancer, particularly squamous cell carcinoma and adenocarcinoma [2]. Hypertrophic osteoarthropathy can also be secondary to a lung abscess, mesothelioma, and other disorders [1].

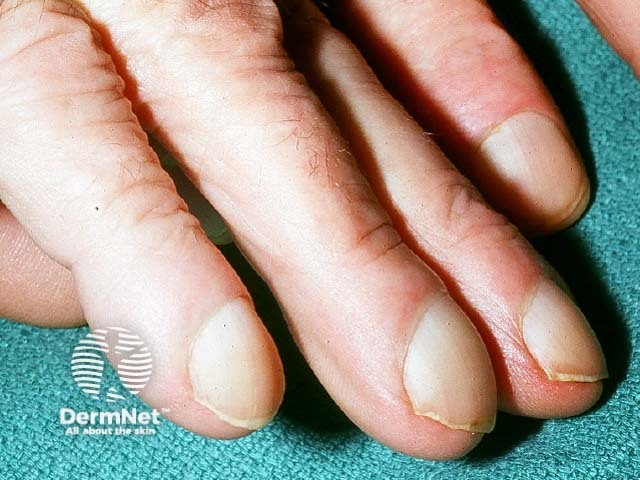
Finger clubbing
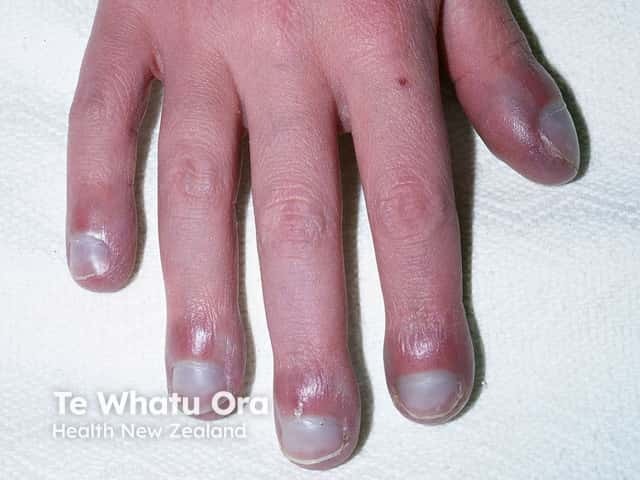
Clubbing of the nails
Cutaneous metastases in lung cancer are found in 2–8% of cases of lung cancer [1]. The most common sites are the chest and abdominal wall, neck, and scalp. They are usually rapidly growing, hard, painless and mobile nodules. A punch biopsy of a nodule may be nonspecific or may establish the diagnosis of lung cancer.
Monitoring changes in the size of skin nodules can help assess the patient's response to chemotherapy [1]. Other cutaneous manifestations of lung cancer include:
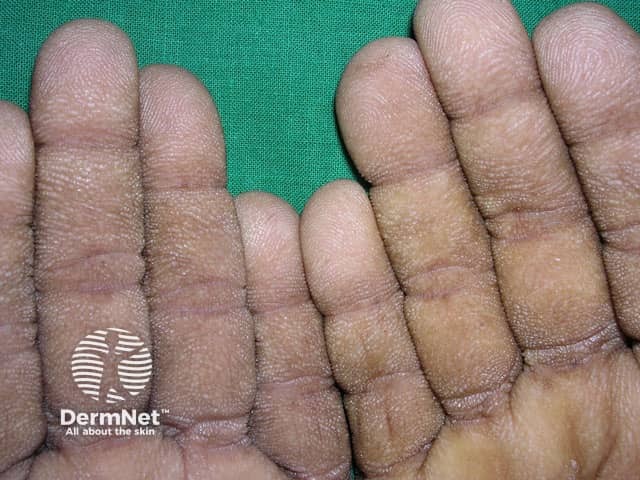
Tripe palms

Thrombophlebitis
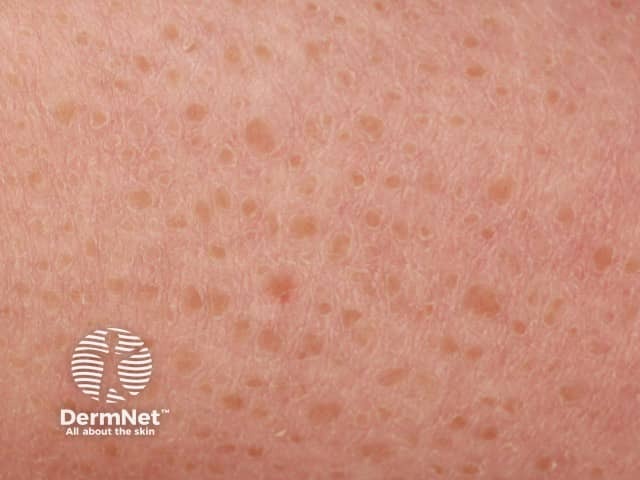
Acquired ichthyosis
Superior vena cava syndrome is due to obstruction of the superior vena cava, the vein that takes deoxygenated blood from the upper body to the heart. The majority of cases are due to malignancy; most commonly, non-small-cell lung cancer, small-cell lung cancer, lymphoma, and metastatic tumours [4]. Superior vena cava syndrome presents with markedly dilated veins or venules in the upper chest [5]. These occur as a result of increased collateral flow through the superficial vasculature in the chest wall.
Sarcoidosis can be divided into two separate conditions:
Cutaneous involvement is classified as either specific, in which there are non-caseating granulomas (mixed chronic inflammatory cells) on histopathology, or nonspecific, in which granulomas are absent.
Specific lesions of sarcoidosis include:
Non–specific lesions of sarcoidosis include:

Lupus pernio
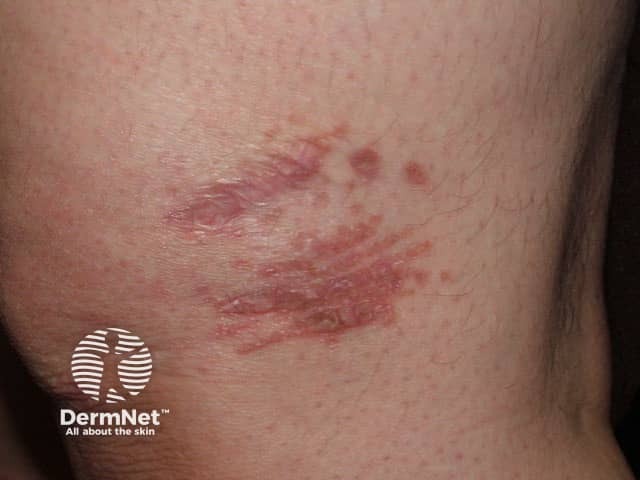
Scar sarcoidosis
Cutaneous manifestations of cystic fibrosis may be nonspecific, but include:

Aquagenic wrinkling of palm (AWP-patient2)
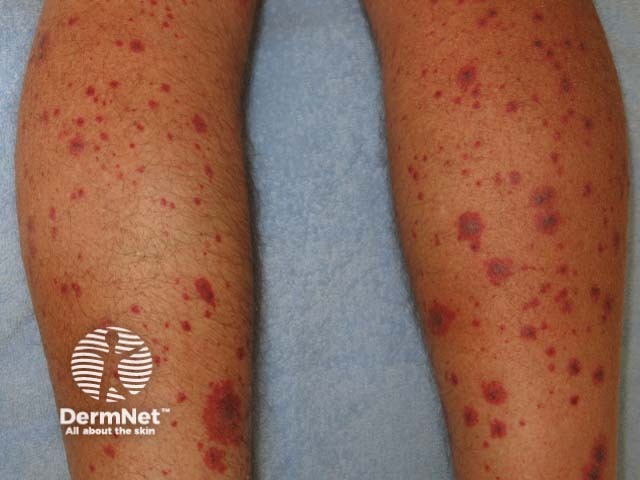
Hypersensitivity vasculitis
Cutaneous manifestations of granulomatosis with polyangiitis (also known as Wegener granulomatosis) are found in 10% of patients at diagnosis and develop in 50% of patients throughout the disease [1,8].
Skin findings include:
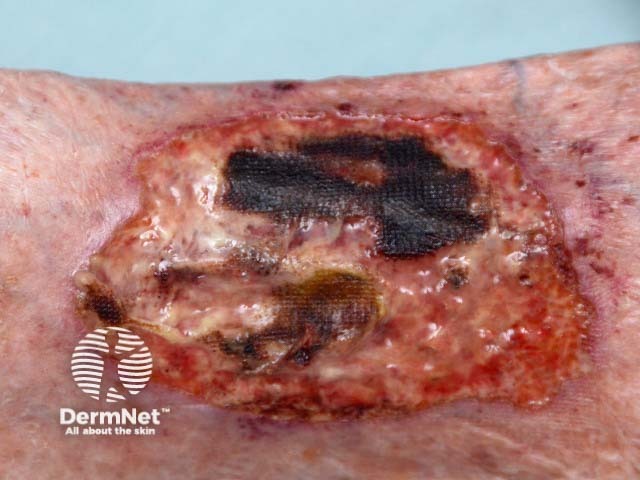
Ulceration
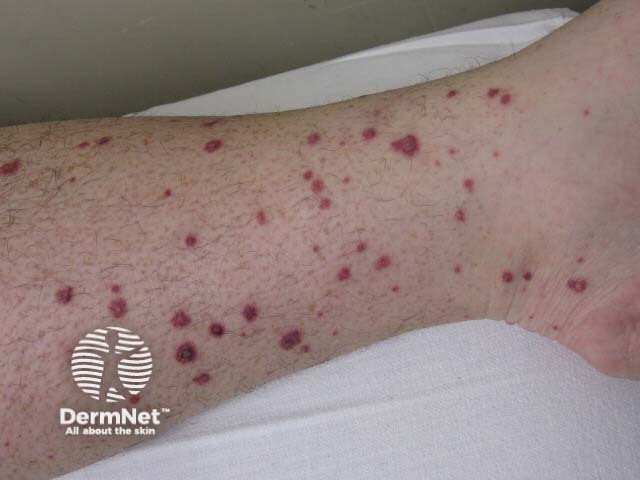
Palpable purpura
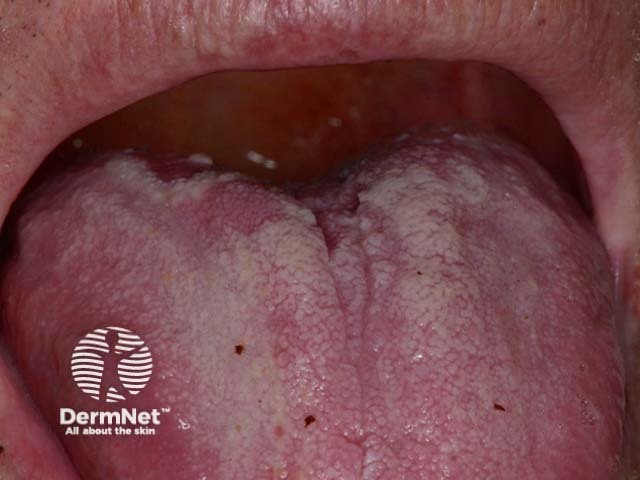
Mouth ulceration and glossitis
Eosinophilic granulomatosis with polyangiitis (also known as Churg-Strauss syndrome) is a rare multisystem disorder that primarily affects the lungs, skin, and peripheral nervous system. The main features are asthma, eosinophil infiltration in the lungs and blood, and small-vessel vasculitis with granulomas on biopsy.
A variety of skin lesions are seen in eosinophilic granulomatosis with polyangiitis:
Papules and nodules may become necrotic, starting with a central black dimple.
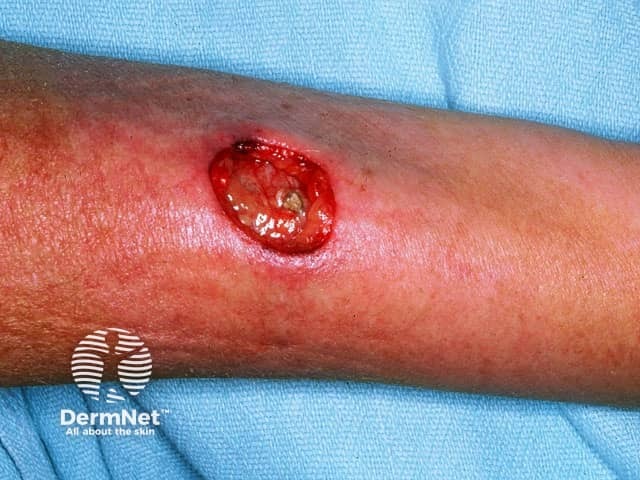
Ulcer
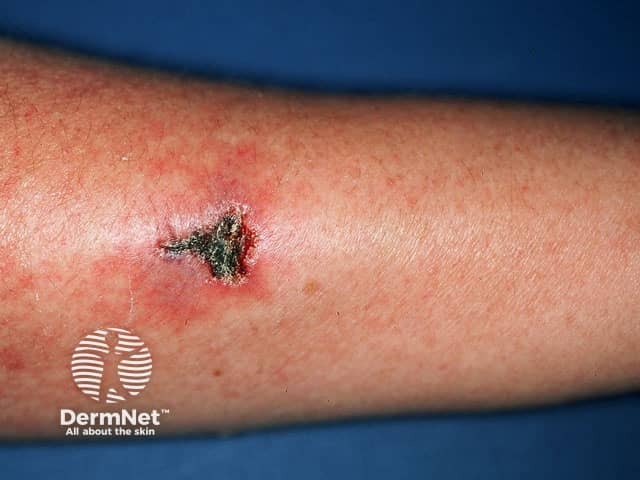
Erythema + eschar
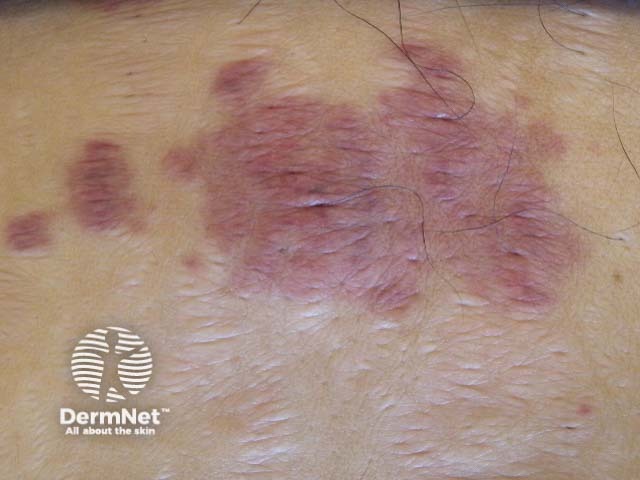
Purpura
Pulmonary arteriovenous malformations are abnormal communications between the arteries and veins that supply the lungs. The majority of these malformations are congenital. Approximately 70% of patients with pulmonary arteriovenous malformations have associated hereditary haemorrhagic telangiectasia (also known as Osler–Weber–Rendu syndrome) in which telangiectasia is near the surface of the skin. The face, hands, feet, chest, lips, tongue, oral mucosa, and nasal mucosa are most commonly affected [1].
Alpha-1-antitrypsin deficiency is a genetic disorder where there is defective production of the alpha-1-antitrypsin enzyme. It primarily affects the lungs (with emphysema), liver, and skin. Cutaneous findings include recurrent ulcerative, necrotising panniculitis (inflamed subcutaneous fat with crops of painful, red subcutaneous nodules), which most noticeably occurs on the trunk and proximal extremities. These nodules typically ulcerate, releasing a clear to yellow oily fluid [1].
Fat embolism syndrome typically follows fractures and trauma to the long bones or pelvis. Fat particles released into the circulation may cause:
The classic cutaneous manifestation of fat embolism syndrome is a petechial eruption with 2–3 mm purpuric macules on non-dependent portions of the body (upper chest, neck, axillae, and conjunctivae). This finding often disappears within 5–7 days, but may be key for diagnosis [10,11].
Yellow nail syndrome is the triad of:
Nail changes that are usually the first features of yellow nail syndrome include:
The nails are occasionally green in colour. Lymphoedema associated with yellow nail syndrome typically affects the legs and is symmetrical and non-pitting.

Yellow nail syndrome
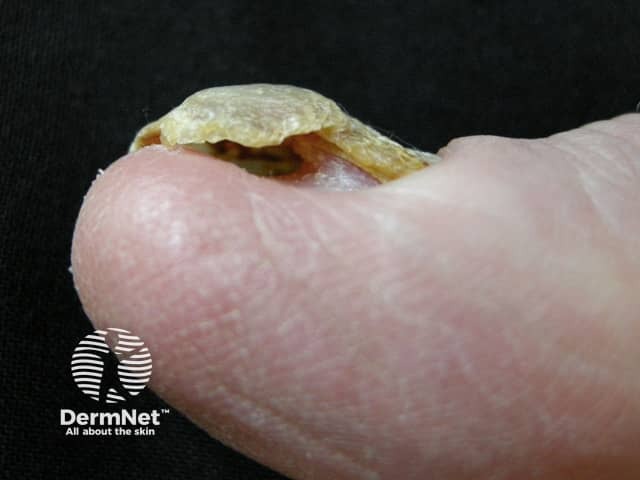
Yellow nail syndrome

Yellow nail syndrome
Birt–Hogg–Dubé syndrome is an autosomal-dominant inherited disease characterised by skin tumours, pneumothorax (lung collapse), kidney tumours, and lung cysts [12].
Cutaneous lesions include:
Fibrofolliculomas and trichodiscomas are most frequently found on the head, face, and upper body.
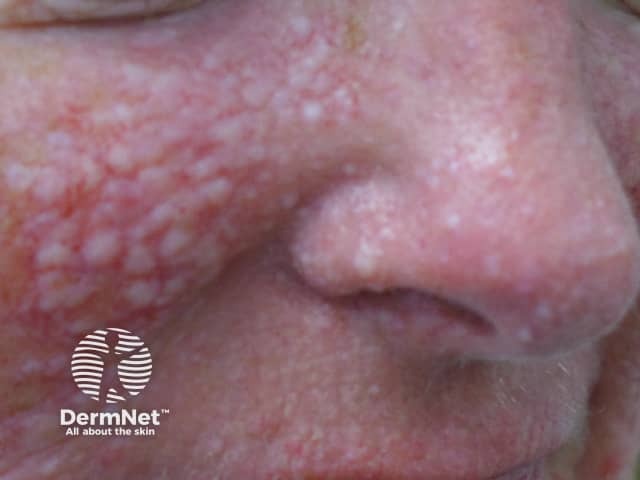
Fibrofolliculomas in Birt Hogg Dube syndrome
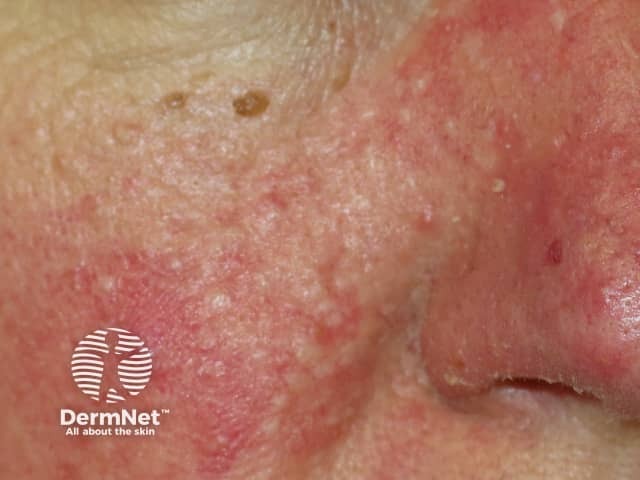
Fibrofolliculomas in Birt Hogg Dube syndrome

Fibrofolliculomas in Birt Hogg Dube syndrome