Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Nicole S Kim, Medical Student, University of Toronto, Canada; Dr Yuliya Velykoredko, Dermatology Resident, University of Toronto, Toronto, Canada. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell/Maria McGivern. September 2018.
Introduction Demographics Causes Clinical features Complications Diagnosis Differential diagnoses Treatment Outcome
Nipple eczema is a localised dermatitis involving the nipple and areola and is characterised by erythema and scaling. It may be itchy and painful. Nipple eczema can be a local manifestation of atopic dermatitis/eczema when it arises with classic age-related patterns of eczema on other body sites, or it can occur in isolation.
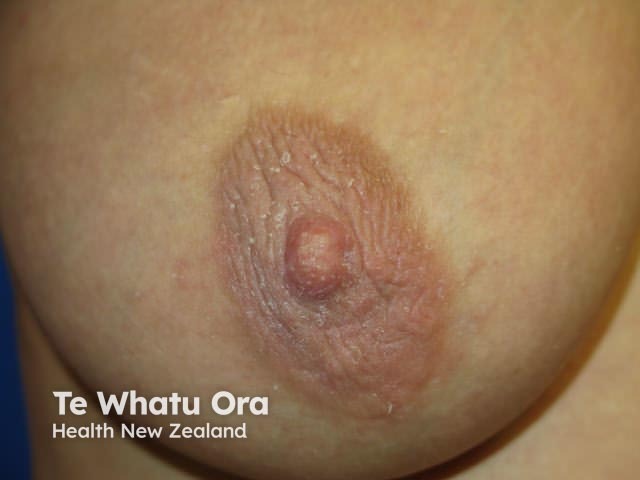
Nipple eczema
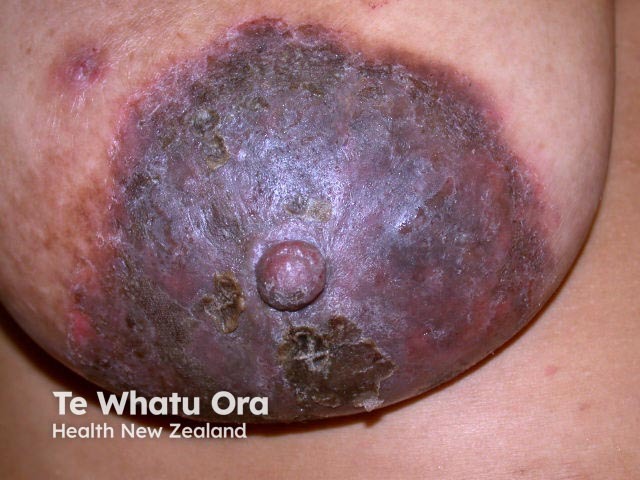
Nipple eczema
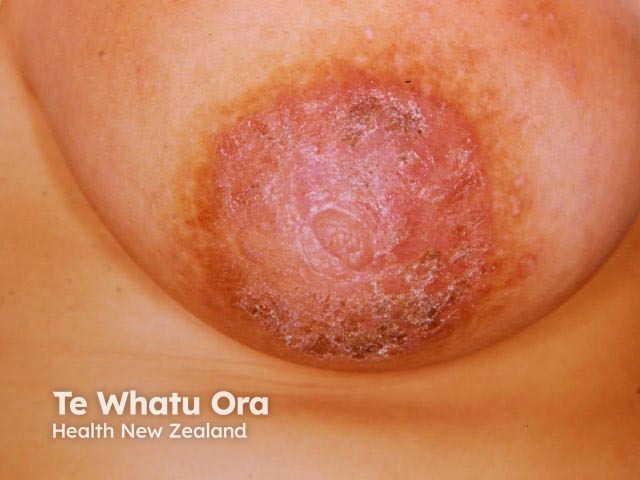
Nipple eczema
Nipple eczema can occur in anyone as a solitary condition; however, it often occurs in patients with current or past eczema elsewhere. Nipple eczema is mostly diagnosed in teenage girls, regardless of any prior history of atopic dermatitis, but it can also affect infants, children, and older men and women. Nipple eczema may occasionally affect non-atopic breastfeeding women [1,2]. [see Lactation and nipple problems]
A genetic predisposition and environmental triggers cause nipple eczema. It occurs in the context of different types of dermatitis, mainly, atopic dermatitis, irritant contact dermatitis, and allergic contact dermatitis.
Nipple eczema most commonly affects the skin of one or both areolae, but the part of the areola at the base of the nipple and the nipple itself are usually spared. Nipple eczema rarely extends into the periareolar skin (around the areola) or to the rest of the breasts.
Acute nipple eczema can present with erythematous papules and plaques, with vesicles, oozing, crusting, or erosions. Chronic nipple eczema has a dry, scaly appearance, with lichenification on an erythematous or hyperpigmented base. Nipple eczema is often itchy and painful, especially in breastfeeding women [3,4].
Secondary bacterial infection may occur, due to fissures and the compromised skin integrity in nipple eczema. Colonisation with Staphylococcus aureus can be further complicated with mastitis or breast abscess if not treated promptly.
Other complications include the rare side effects associated with the therapeutic agents used for nipple eczema, such as atrophy from the excessive use of potent corticosteroids or folliculitis from an occlusive emollient [3,4].
The diagnosis of nipple eczema is made clinically. Occasionally, other tests may be required.
Other conditions that should be considered in a patient with nipple eczema include:
A diagnosis of allergic contact dermatitis should be considered if there is a minimal response to conventional treatment methods for nipple eczema, especially in patients with bilateral lesions extending beyond the areola. Mammary Paget disease, a slow-growing cutaneous form of intraductal carcinoma, should be ruled out in an adult with a unilateral and chronic eczematous lesion of the nipple persisting for more than three months that has not improved after using a topical steroid.
Other rarer conditions that may be mistaken for nipple eczema include erosive adenomatosis, psoriasis, Hailey–Hailey disease, and pemphigus. Skin cancers (eg, intraepidermal squamous cell carcinoma, basal cell carcinoma, and malignant melanoma) should be ruled out when there is a reasonable degree of suspicion [4].
The multifactorial causes of nipple eczema should be addressed. The prevention of recurrence is key, and patients should be encouraged to avoid precipitating irritants and allergens where these are known. Routine skin care should include moisturisers, as these will help restore the skin’s normal barrier function and reduce pain and itch [3,4].
Topical corticosteroids (especially in ointment formulation) are the mainstay of treatment for most cases of nipple eczema. They work well and are easily absorbed by the thin areolar skin.
In breastfeeding women with nipple eczema, topical steroids should be applied after breastfeeding the infant. Before nursing, these should be then wiped off to avoid potential steroid-related adverse effects by expressing breast milk from the breast and using it to wipe off the steroid ointment; the fat contained in the milk may help retain moisture in the nipple and minimise dryness.
Systemic steroids are rarely necessary for eczema confined to the nipple or the skin of the breast.
Topical calcineurin inhibitors (eg, tacrolimus and pimecrolimus) are also useful, but there is little information in the literature about the potential side effects on the breastfed infant.
Secondary bacterial skin infection (S. aureus) should be treated with antibiotics. Systemic antibiotics have shown better eradication of infection compared to topical antibiotics; they are also less likely to induce methicillin-resistant bacteria and are less likely to result in antibiotic allergy [3].
Pain or burning discomfort of the nipples can be relieved by taking paracetamol; this is generally safe in a breastfeeding mother [1,4].
Nipple eczema tends to run a chronic course with varying degrees of relapse and remission. The aim is to prevent exacerbations by identifying and avoiding precipitating factors.
Patients should be educated on basic skin care. Mild nipple eczema can generally be well-controlled with the avoidance of soap, the application of liberal emollients, and the intermittent application of a topical steroid when the eczema is active [3,4].