Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Amy Stanway, Dermatology Registrar, Waikato Hospital, Hamilton, New Zealand, 2002. Updated by A/Prof Amanda Oakley, February 2016.
Introduction Classification Clinical features Diagnosis Treatment Outcome
Panniculitis refers to a group of conditions that involve inflammation of subcutaneous fat. Despite having very diverse causes, most forms of panniculitis have the same clinical appearance. The diagnosis is established by a skin biopsy, as there are characteristic microscopic features depending on the cause. The most common form of panniculitis is erythema nodosum.
Panniculitis is classified as mostly septal panniculitis or mostly lobular panniculitis depending on the site of the most intense microscopic inflammation. Most types of panniculitis have both septal inflammation (early) and lobular inflammation (later). Further classification is based on whether or not there is subcutaneous vasculitis, and the type of inflammation noted (neutrophils, lymphocytes, histiocytes, granulomas).
Panniculitis presents typically with:
Sometimes, lesions resolve to leave localised subcutaneous atrophy (lipodystrophy).
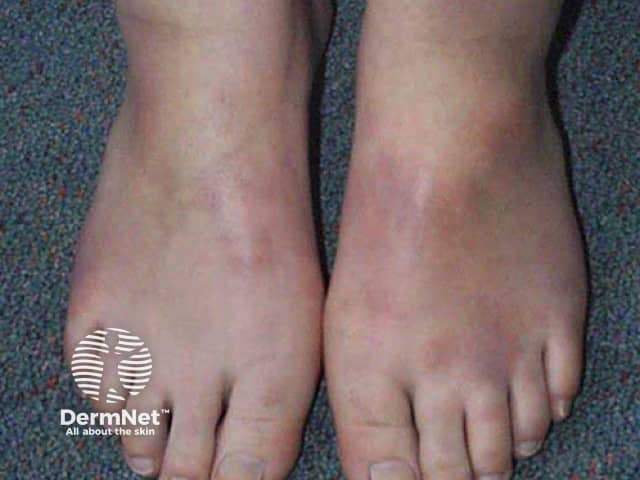
Panniculitis
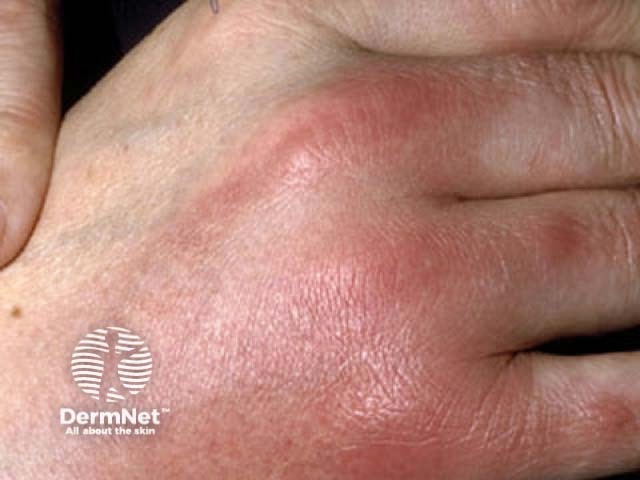
Panniculitis
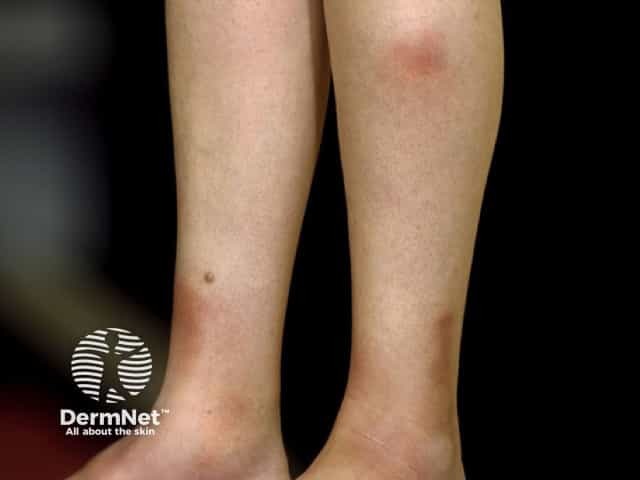
Erythema nodosum
Associated symptoms of fever, malaise and arthralgia are common in patients with panniculitis. When these are prominent, diagnoses to consider include:
Panniculitis is diagnosed and classified by a combination of clinical features, biopsy findings and microbiological culture. Sometimes other investigations are necessary (such as chest X-ray in erythema nodosum and alpha-1-antitrypsin levels).
The histopathology may show the inflammation to be lobular, septal or mixed, with or without vascular damage, and predominantly neutrophils, lymphocytes or granulomatous.
Treatment of panniculitis includes:
The outcome depends on the underlying cause of the inflammation. After an inflammatory phase of weeks to months, panniculitis often settles down. It may recur. Some forms of panniculitis do not leave a mark, but destructive forms of panniculitis tend to leave a permanent dent in the skin.
Medscape Reference: