Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Katherine Allnutt, Research and Education Fellow, Skin and Cancer Foundation Inc, Melbourne, VIC, Australia. DermNet Editor in Chief: Adjunct A/Prof. Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell/Maria McGivern. December 2018.
Introduction Demographics Causes Clinical features Diagnosis Differential diagnoses Treatment Outcome
Periorificial dermatitis in children typically presents as multiple small papules around the mouth, nose, and eyes.
While the name is suggestive of an eczematous condition, periorificial dermatitis is actually more like rosacea.
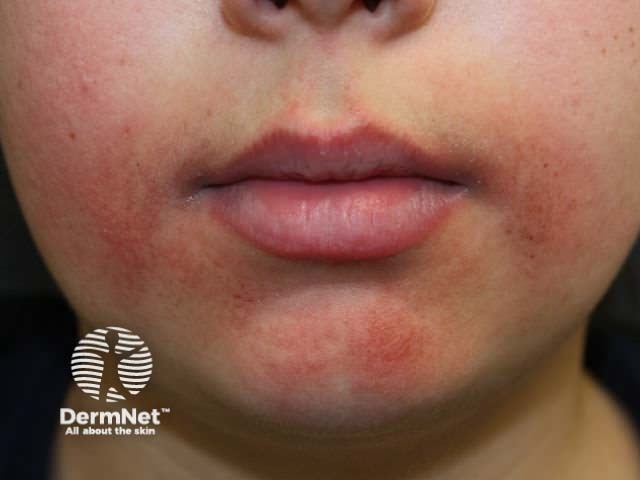
Periorificial dermatitis
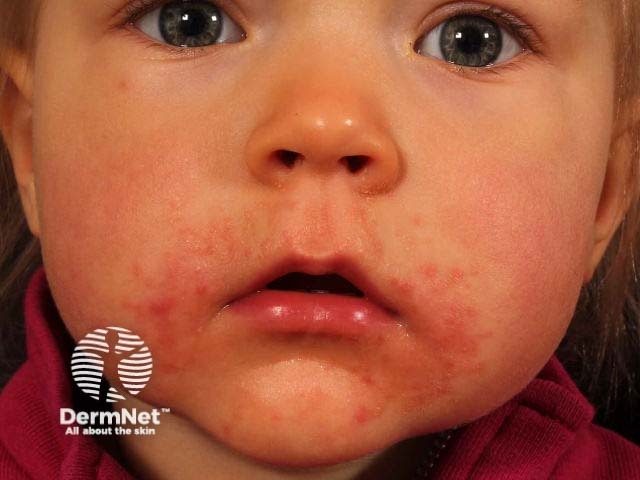
Periorificial dermatitis in a child
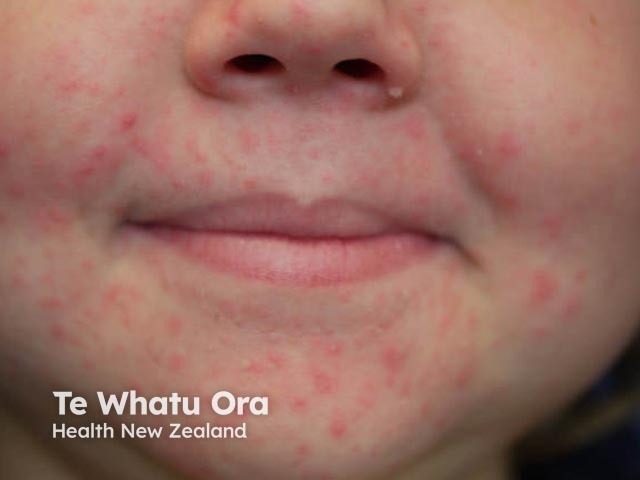
Periorificial dermatitis in a child
Periorificial dermatitis mostly affects women aged 16–45 years; it is less common in men [1,2]. It can also affect children as young as 3 months of age, with the average age of children being 6.6 years [3]. Periorificial dermatitis is slightly more common in girls than in boys and is seen most frequently in children who have had topical steroids to the face [3,4].
The cause of periorificial dermatitis is poorly understood.
Periorificial dermatitis is characterised by multiple grouped erythematous papules, pustules, or vesicles, with or without any scale.
Granulomatous periorificial dermatitis is a variant mainly reported in dark-skinned prepubertal children in which there are multiple small discrete flesh-coloured or hyperpigmented papules. Granulomatous periorificial dermatitis is mainly reported in dark-skinned prepubertal children.
Periorificial dermatitis is usually diagnosed from a typical patient history and clinical features.
A skin biopsy is rarely required but may distinguish periorificial dermatitis from other disorders when the diagnosis is unclear.
Swabs, skin scrapings, and potassium hydroxide preparation may exclude bacterial or fungal infection.
Patch testing may be indicated if a contact allergy is suspected.
Blood tests are not useful in the diagnosis of periorificial dermatitis.
The differential diagnosis for non-granulomatous periorificial dermatitis in prepubertal children includes [11,18]:
In older children, the following conditions should also be considered:
The differential diagnosis for the granulomatous variant includes [18]:
Suspected causative agents, such as topical corticosteroids, should be discontinued [1].
Mild periorificial dermatitis may be treated with a topical antibiotic, such as metronidazole, clindamycin, erythromycin and sulfacetamide [3,4,11,19]. Clearance typically takes 3 to 8 weeks [11].
Refractory or moderate to severe disease is treated with oral antibiotics.
Other treatments reported to be effective for periorificial dermatitis include:
Periorificial dermatitis in children is generally benign and self-limiting and often improves spontaneously within 2–3 weeks.