Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Anoma Ranaweera, Medical Writer, Auckland, New Zealand, 2012.
Introduction
Clinical features
Risk factors
General management
Radiation dermatitis is a side effect of external beam ionizing radiation. It is also called radiodermatitis, x-ray dermatitis, radiation skin damage or a radiation burn.
Most commonly, radiation-induced dermatitis is caused by radiotherapy for underlying malignancies. It may also rarely result from exposure to radiation during interventional procedures such as coronary angiography, embolization procedures, and indwelling catheter placements.
Irradiation of the skin leads to a complex pattern of direct tissue injury involving damage to cells of the epidermis and endothelial cells within the walls of blood vessels, and inflammatory cell recruitment.
Radiation dermatitis generally manifests within a few days to weeks after the start of radiotherapy. Its onset varies depending on the radiation dose intensity and the normal tissue sensitivity of individuals. It is confined to areas of skin that have been irradiated, and the skin changes are sharply demarcated.
Radiation-induced dermatitis can be classified as acute or chronic.
Acute radiation dermatitis occurs within 90 days of exposure to radiation. The patient may have skin changes ranging from faint erythema (reddening) and desquamation (peeling skin) to skin necrosis (death of skin cells) and ulceration, depending on the severity of the reaction.
The National Cancer Institute (USA) has developed 4 criteria for the classification of acute radiation dermatitis:
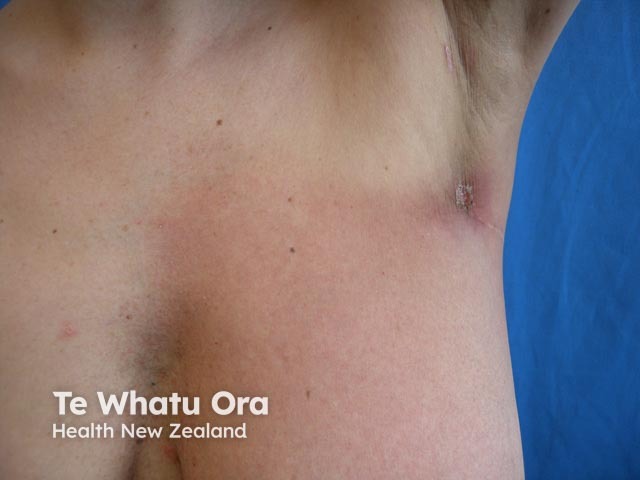
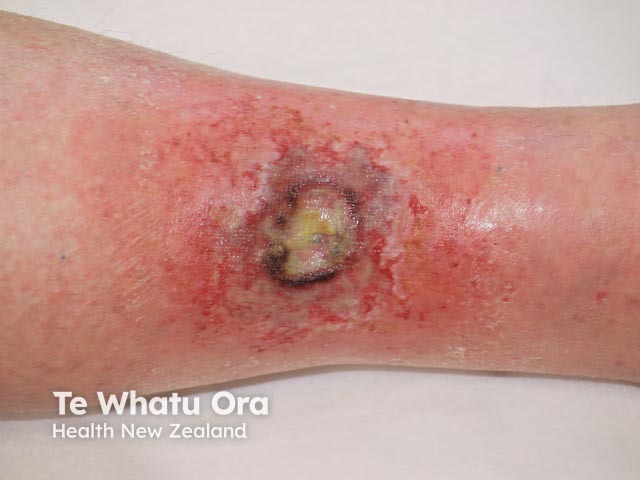
Acute radiation dermatitis
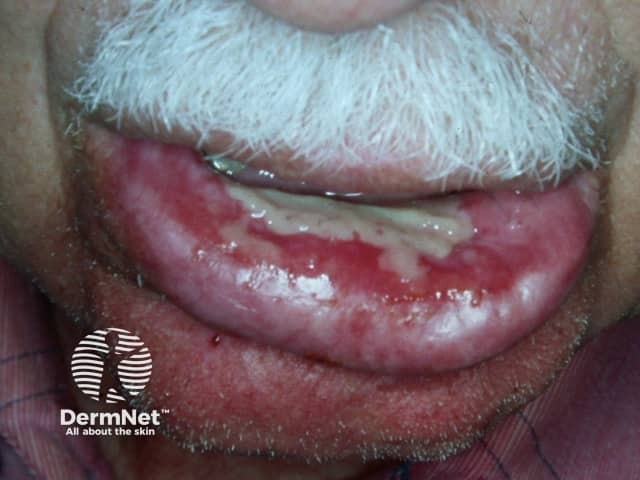
Radiation-induced stomatitis
The onset of chronic radiation dermatitis may occur from 15 days to 10 years or more after the beginning of radiation therapy. It is an extension of the acute process and involves further inflammatory changes in the skin.
Chronic radiation-induced changes in the skin are characterised by:
Secondary skin cancers may also result from repeated exposure to radiation therapy, most commonly basal cell carcinoma.
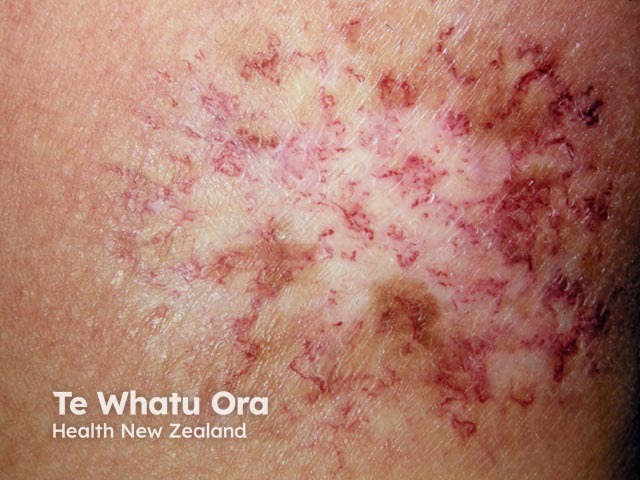
Chronic radiation dermatitis
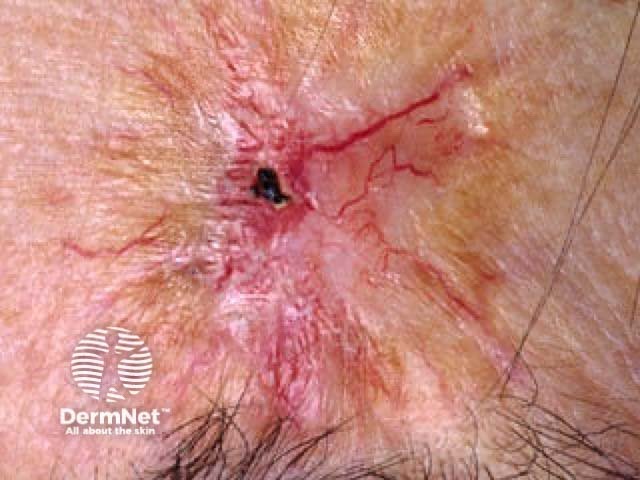
Chronic radiation dermatitis
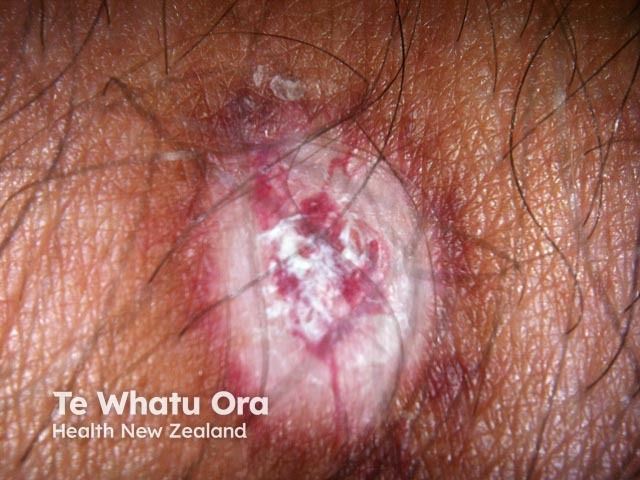
Chronic radiation dermatitis
Radiation recall is rare. It occurs at sites of previous radiation therapy after a chemotherapy agent (e.g. methotrexate or etoposide) is given. The reaction may occur weeks to years after radiation.
Radiation recall ranges from sunburn-like erythema to necrosis, ulceration, and bleeding.
Radiation-induced dermatitis is more likely to occur in patients with certain risk factors:
Certain diseases and syndromes increase the risk of radiation dermatitis. These include:
Patients with acute radiation dermatitis should be carefully assessed.
Patients may wash the affected skin with a gentle non-soap cleanser and dry it with a soft, clean towel before each irradiation session. Emollients, moisturisers, gels, emulsions and dressings applied after treatment may reduce discomfort.
Topical corticosteroids may be prescribed for radiation dermatitis for 2 to 4 weeks. It is uncertain whether these are of benefit.
Patients receiving radiation therapy should be advised to avoid: