Introduction
Dermatological symptoms and signs sometimes precede or accompany a gastrointestinal disease. It should be noted that the embryonic origin of the gastrointestinal tract and the skin are closely aligned.
Liver cirrhosis
Common cutaneous manifestations of liver cirrhosis include:
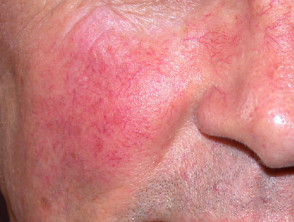
- Telangiectases
- Spider telangiectasis
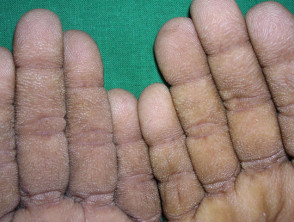
- Palmar erythema
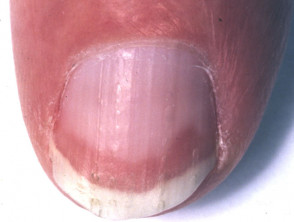
- Terry nails (82%): white proximal (leukonychia) and pink distal nail plate.
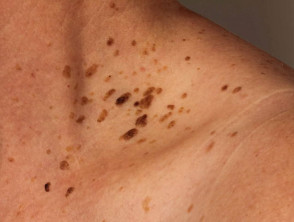
- Haemochromatosis: an autosomal dominant iron-accumulation disorder that may cause generalised bronze hyperpigmentation
- Wilson disease: an autosomal recessive disorder of copper metabolism. Signs of Wilson disease include:
- Kayser-Fleischer ring around iris
- Pigmentation over the shins
- Blue lunulae (half-moons) on nails.
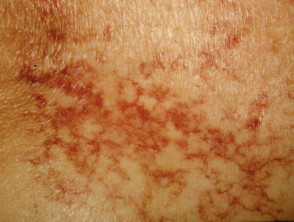
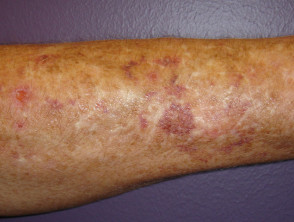
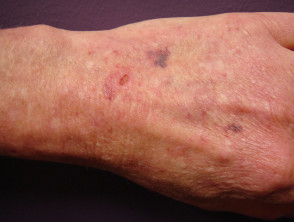
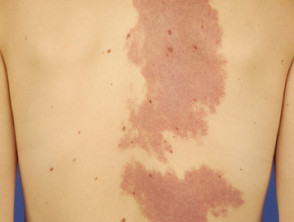
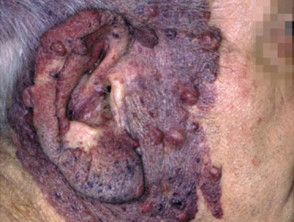
Cutaneous effects of liver disease
Nutritional and metabolic disorders
Nutritional deficiency
Malnutrition associated with deficiencies of fat-soluble and water-soluble vitamins often affects the skin.
Fat-soluble vitamins:
- Vitamin A deficiency causes phrynoderma, ie keratotic follicular papules on anterolateral thighs and posterolateral upper arms.
- Vitamin D deficiency in babies and children results in delayed tooth eruption with poor enamel. In adults, it predisposes to caries.
- Vitamin K deficiency affects coagulation, leading to haemorrhage, purpura and ecchymoses.
Water-soluble vitamins:
- Acute vitamin B2 deficiency results in:
- Deep red erythema
- Stomatitis
- Epidermal necrolysis (peeling skin)
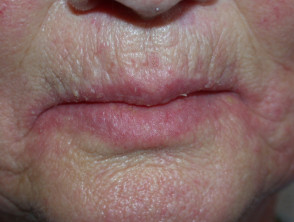
- Chronic vitamin B2 deficiency causes:
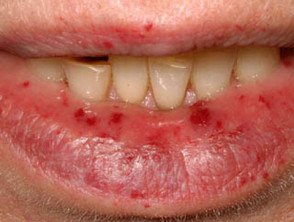
- Angular cheilitis
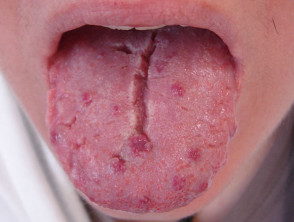
- Prominent lingual papillae (papules on the tongue)
- Seborrhoeic dermatitis
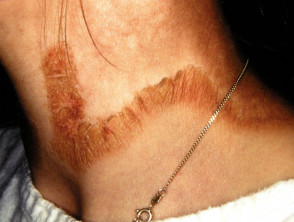
- Vitamin B3 deficiency causes pellagra, characterised by:
- Photosensitivity
- Casal necklace – rash distributed around neck/upper chest
- Cheilitis, glossitis (inflamed tongue), angular cheilitis, oral or perirectal ulcers
- Vitamin B6 deficiency causes:
- Seborrhoeic dermatitis-like eruption
- Glossitis
- Angular cheilitis
- Vitamin B9/B12 deficiency is associated with:
- Angular cheilitis
- Hunter glossitis (atrophic, red and painful tongue)
- Hair depigmentation
- Hyperpigmentation (diffuse and symmetrical pigmentation, hands, nails, face, palmar creases, flexural regions and pressure points)
- Vitamin C deficiency causes scurvy, characterised by:
- Enlarged, hyperkeratotic hair follicles on posterolateral aspects of arms
- Abnormal hair development
- Swelling of gums, erythema
- Splinter haemorrhage in nails
- Biotin deficiency results in:
- Periorificial dermatitis
- Alopecia
- Intertrigo and seborrhoeic erythroderma
Skin signs of vitamin deficiency
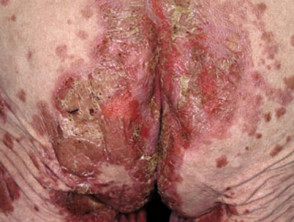
Acrodermatitis enteropathica
Acrodermatitis enteropathica is an autosomal recessive inherited form of zinc deficiency that manifests in infancy. It presents with the clinical triad of dermatitis, alopecia and diarrhoea. Skin signs include:
- Pink, scaly patches and plaques on extremities, periorificial and anogenital sites
- Can include psoriasiform plaques, vesicular, bullous, pustular or erosive lesions.
- Hair loss may follow.
See also Acrodermatitis enteropathica-like conditions.
Eruptive xanthomas
Eruptive xanthomas are:
- Caused by the accumulation of fat in macrophage cells in the skin
- Associated with hypertriglyceridaemia, often due to diabetes mellitus
Eruptive xanthomas
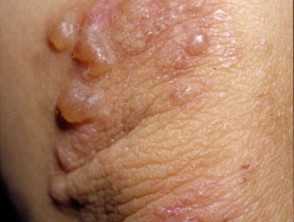
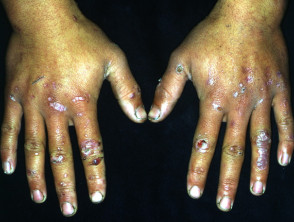
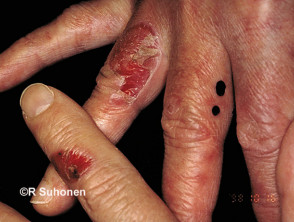
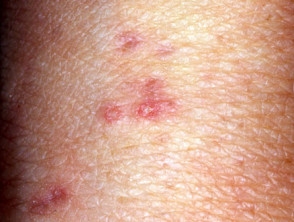
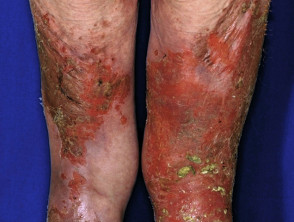
Dermatitis herpetiformis
Dermatitis herpetiformis is associated with:
- Human leukocyte antigens (HLA) DQ2 or DQ8
- Gluten-sensitive enteropathy (coeliac disease) with villous atrophy of duodenum
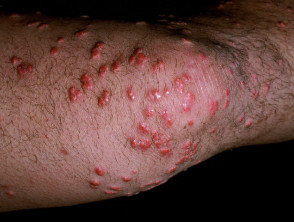
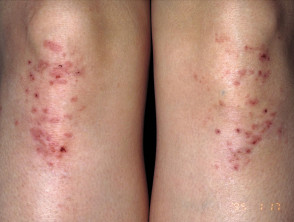
Skin signs of dermatitis herpetiformis include:
- Intensely itchy herpetiform vesicles within erythematous or urticated plaques
- Excoriated erythematous, crusted, grouped papules
- Symmetrical distribution on extensor surfaces: elbows, knees, shoulders and buttocks
Dermatitis herpetiformis
Inflammatory bowel disease
Inflammatory bowel disease (IBD) refers to ulcerative colitis and Crohn disease. There are similarities and differences in their cutaneous manifestations.
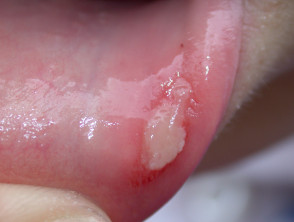
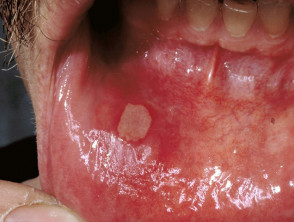
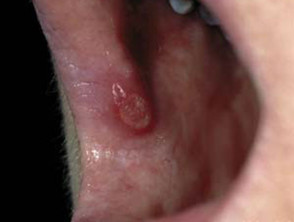
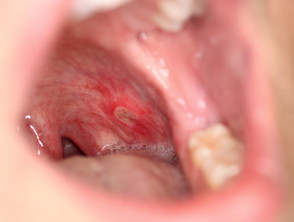
Oral aphthous ulcers
Aphthous ulcers are common in both forms of inflammatory bowel disease.
- Round, oedematous mucosal ulcers
- Sometimes associated with nutritional deficiencies
Aphthous ulceration
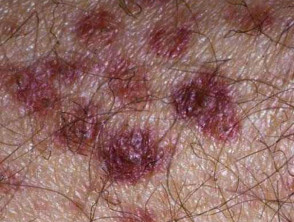
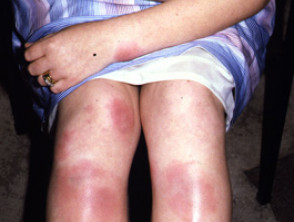
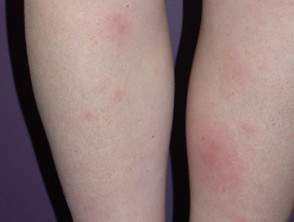
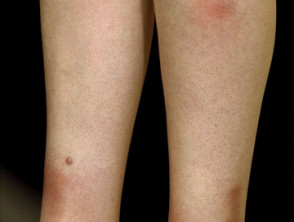
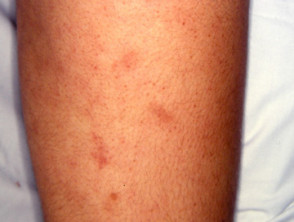
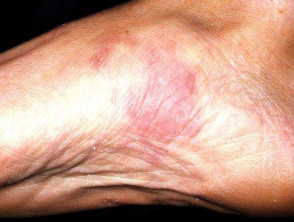
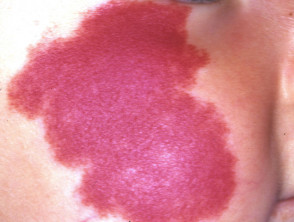
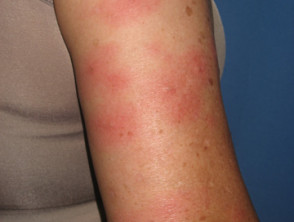
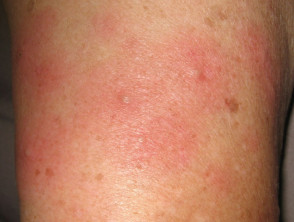
Erythema nodosum
Erythema nodosum (EN) is the most common skin sign of Crohn disease (4-6%) or ulcerative colitis (3%).
- A form of panniculitis
- Tender red subcutaneous nodules
- Mostly on symmetrical extensor surfaces of lower legs
- Can be found on thighs, extensor surfaces of arms, trunk and face
Erythema nodosum
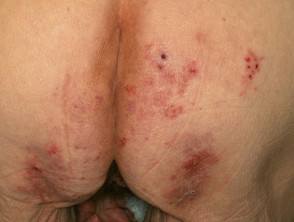
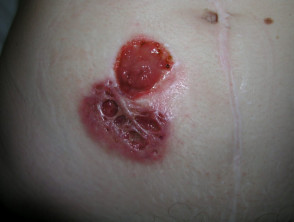
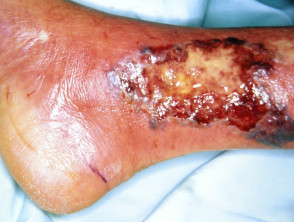
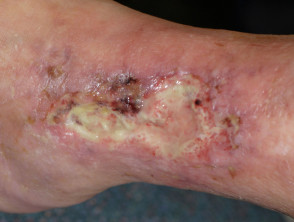
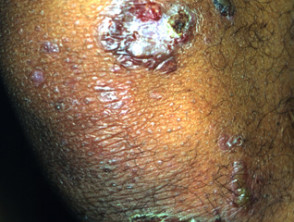
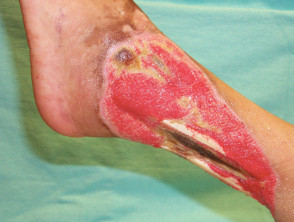
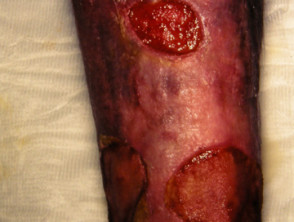
Pyoderma gangrenosum
Pyoderma gangrenosum (PG) affects 0.7% of patients with Crohn disease and 2% with ulcerative colitis.
- Ulcers with irregular undermined or overhanging necrotic borders
- Usually affects lower extremities but may arise anywhere
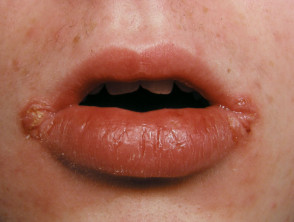
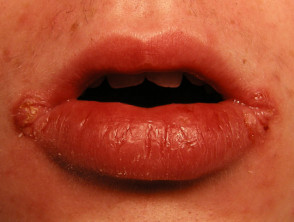
- Peristomal PG develops two months to 25 years after stoma creation
- Associated with pyostomatitis vegetans: pustules and ulcers on lips and buccal mucosa.
Pyoderma gangrenosum
Perianal fissure/fistulae
Fissures and fistulae are common in Crohn disease (36%) and do not occur in ulcerative colitis.
- Multiple circumferential fissures/fistulae
Swelling of oral cavity/labia
Mucosal oedema affects 8–9% of patients with Crohn disease and is absent in ulcerative colitis.
- Frequently painful and disruptive to eating
Metastatic Crohn disease
Metastatic Crohn disease may cause cutaneous granulomatous plaques, nodules and ulcers.
- Affects extremities or intertriginous areas
- Facial and genital lesions are rare
Skin complications of Crohn disease
Epidermolysis bullosa acquisita (EBA)
Epidermolysis bullosa acquisita (EBA) is a rare immunobullous disorder sometimes associated with Crohn disease.
Epidermolysis bullosa acquisita
Cutaneous polyarteritis nodosa
Cutaneous polyarteritis nodosa is a rare form of necrotising, small and medium-sized vasculitis.
- 10% of cases are associated with IBD
- Causes tender arterial nodules, palpable purpura and ulceration
- Mainly affects lower extremities
Cutaneous polyarteritis nodosa
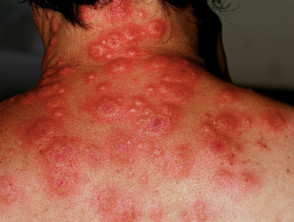
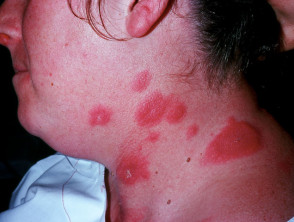
Acute neutrophilic dermatosis
Acute neutrophilic dermatosis, also known as Sweet syndrome, is an autoinflammatory disorder sometimes associated with inflammatory bowel disease. Features include:
- Fever and malaise
- Cutaneous and mucosal involvement
- Tender, oedematous erythematous papules and plaques
- Vesicles, bullae or pustules within the plaques
- Typically affects the head, neck and extremities but can be widespread
- Usually resolves spontaneously within 5–12 weeks
Acute febrile neutrophilic dermatosis
Vascular disorders
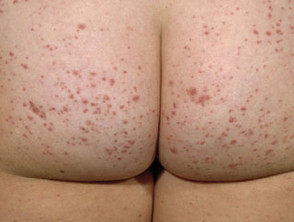
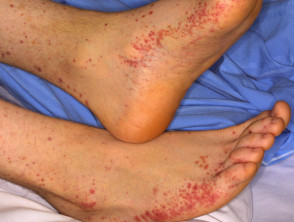
Henoch-Schönlein purpura
Henoch-Schönlein purpura (HSP) is an immunoglobulin A-mediated, leukocytoclastic, small-vessel vasculitis.
- Palpable purpuric lesions usually affect buttocks and legs.
- HSP may also cause gastrointestinal vasculitis causing abdominal pain and melaena, due to bowel wall oedema, haemorrhage, and rarely, bowel infarction, perforation and intussusception.
- Other symptoms may include arthritis (80%), abdominal pain (50–75%) and nephritis (40%).
Henoch Schönlein purpura
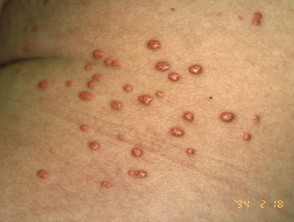
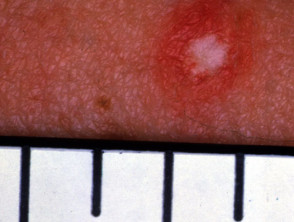
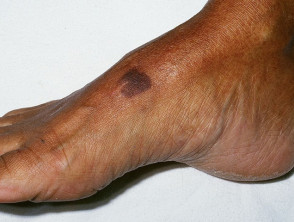
Degos disease
Degos disease is small vessel angiopathy, thought to be due to dysregulation of interferon-alfa and the membranolytic attack complex. There are two variants: benign atrophic papulosis and malignant atrophic papulosis.
- Degos disease presents with 2–5 mm, rose-coloured papules that heal as umbilicated scars with white porcelain centre, erythematous rim, and surrounding telangiectasia.
- Lesions most commonly occur on the trunk and arms, sparing the face, palms and soles.
- Malignant atrophic papulosis is associated with gastrointestinal disease in 50–61%, causing intestinal perforation. Plaques are found on serosa and peritoneum.
Malignant atrophic papulosis
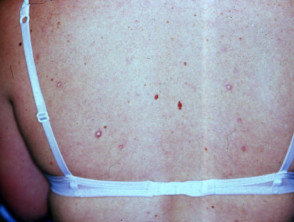
Hereditary haemorrhagic telangiectasia
Hereditary haemorrhagic telangiectasia (HHT) is a hereditary, autosomal dominant, bleeding disorder.
- Multiple, small punctate telangiectases affect 50% of patients by 30 years of age.
- Telangiectases are predominantly found on face and mouth.
- Recurrent nosebleeds affect 90% of patients with HHT.
- Bleeding may also occur from gastrointestinal arteriovenous malformations.
Hereditary haemorrhagic telangiectasia
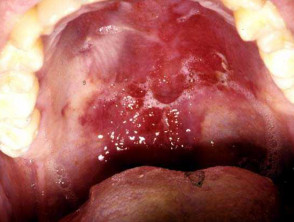
Kaposi sarcoma
Kaposi sarcoma (KS) is a human herpesvirus 8-associated tumour of endothelial cells.
- It presents with pink, red, brown or violaceous macules, papules, nodules or plaques.
- These most often arise on lower extremities or head and neck.
- KS often affects oropharynx, presenting as one or more violaceous stains on the hard palate.
Kaposi sarcoma
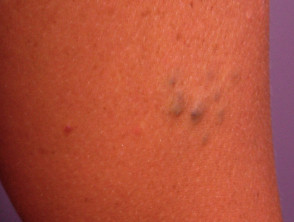
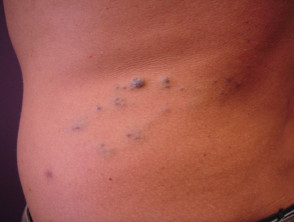
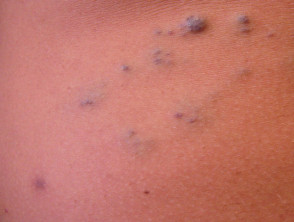
Blue rubber bleb naevus syndrome
Blue rubber bleb naevi are venous malformations of skin and gastrointestinal tract.
- They may form anywhere from the mouth to the anus, most commonly in the small bowel.
- The “blue rubber nipple” is a blue-purple, soft, rubbery subcutaneous nodule that fills after compression.
- Associated haemangiomas are tender macular lesions found on upper limbs, trunk, perineum.
Blue rubber bleb naevus syndrome
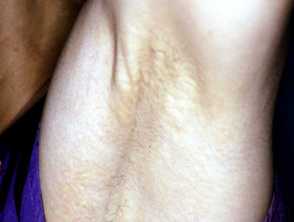
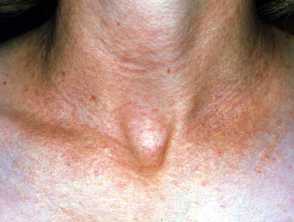
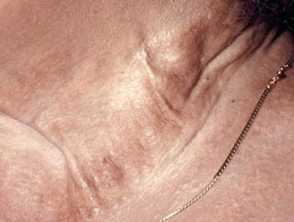
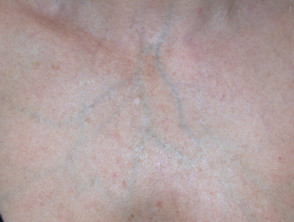
Pseudoxanthoma elasticum
Pseudoxanthoma elasticum (PXE) is an inherited disease in which there are calcification and fragmentation of elastin fibres in the skin and internal organs.
- It presents in early teens with cutaneous changes.
- Small yellow papules coalescing into cobblestone plaques are found on neck, flexures, bottom lip and are associated with loss of cutaneous elasticity.
- Gastrointestinal haemorrhage affects 15% of patients.
Pseudoxanthoma elasticum
Ehlers-Danlos syndrome type IV
Ehlers-Danlos syndrome (EDS) type IV is an inheritable connective tissue disease due to a defect in collagen synthesis.
- Patients present with translucent skin, varicosities, delayed wound healing and keloids.
- They are susceptible to arterial rupture and visceral perforation.
Ehlers-Danlos syndrome
Klippel-Trenaunay syndrome
Klippel–Trénaunay syndrome presents in infancy with a cutaneous capillary vascular malformation.
- Vascular lesions start as salmon pink patches that deepen in colour and thickness over time.
- Extensive varicose veins may lead to chronic venous insufficiency and lymphoedema.
- Gastrointestinal involvement includes vascular malformation in jejunum, distal colon and rectum, and oesophageal varices.
- Bony and soft tissue hypertrophy are common.
Capillary vascular malformations
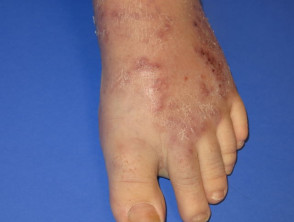
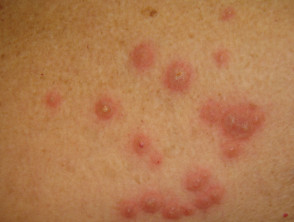
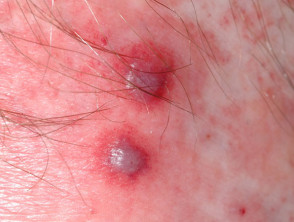
Bowel-associated dermatosis-arthritis syndrome
Bowel-associated dermatosis-arthritis syndrome (BADAS, bowel bypass syndrome) presents with recurrent and episodic flu-like symptoms, polyarthralgia and cutaneous lesions.
- BADAS is thought to be driven by the overgrowth of bacteria in areas of an altered gastrointestinal tract, following surgery or inflammation.
- Skin signs include:
- Erythematous macules rapidly evolve into vesiculopustules and inflammatory papules. These regress over about a week.
- Mainly found on extremities and upper trunk
- Flares every 4–6 weeks
Skin rash associated with bowel bypass syndrome
Hermansky-Pudlak syndrome
Hermansky-Pudlak syndrome is a form of tyrosine-positive oculocutaneous albinism with autosomal recessive inheritance.
- Pigment dilution of skin, hair and eyes is noted at birth.
- Hermansky-Pudlak syndrome is rare outside Puerto Rico.
- It is associated with granulomatous colitis.
Hereditary gastrointestinal tumours
Familial adenomatous polyposis
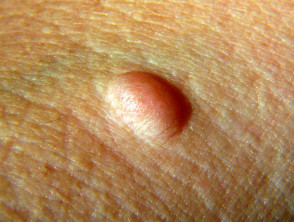
Gardner syndrome is a variant of familial adenomatous polyposis with numerous adenomatous polyps and mucocutaneous findings, such as:
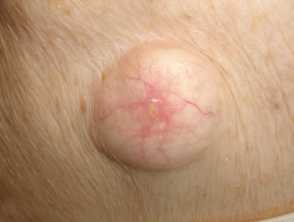
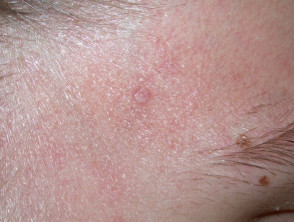
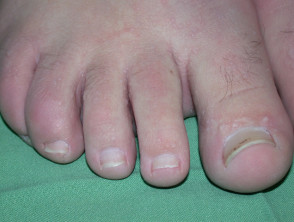
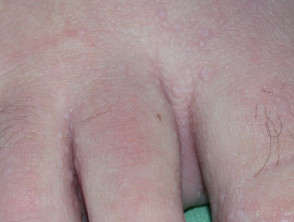
- Epidermoid cysts on face or extremities.
- Lipomas
- Desmoid tumours (10-14%), which are benign fibrous mesenchymal neoplasms. They are non-tender, well-circumscribed, firm, flesh coloured tumours located on the abdomen; intra-, extra- and within the abdominal wall. They can also occur on the shoulder, chest wall and inguinal area.
Skin lesions that might be associated with Gardner syndrome
Hereditary nonpolyposis colorectal cancer
Hereditary nonpolyposis colorectal cancer, also known as Lynch syndrome, is the most common hereditary cancer.
- is an autosomal dominant disorder, accounting for 3% of all colon cancers
- Muir-Torre variant has most of the skin manifestations:
- Sebaceous adenoma and sebaceoma: yellow papules or nodules usually on the face
- Sebaceous carcinoma, a periorbital or extraocular yellow nodule that may ulcerate and invade
- Multiple keratoacanthomas and cutaneous squamous cell carcinomas.
Peutz-Jeghers syndrome
Peutz-Jeghers syndrome is a hamartomatous polyposis syndrome with autosomal dominant inheritance.
- Mucocutaneous pigmentation affects 95%, with small melanocytic macules (lentigines) that appear during childhood.
- The lentigines cluster around the mouth, nostrils, eyes, digits, hands, feet, and perianal region.
- Facial lentigines may fade in adult life; oral-buccal pigmentation is usually permanent.
Cowden syndrome
Cowden syndrome, or multiple hamartoma syndrome, is characterised by skin lesions and polyposis coli.
Trichilemmomas are benign hamartomas of the outer sheath of hair follicles. They are:
- Flesh-coloured, smooth papules
- 1–5 mm in size
- Predominantly on face, head, neck and hairline
Other skin lesions described in Cowden syndrome include:
- Benign papillomas on the face, oral mucosa and acral surfaces
- Cobblestone appearance within the mouth
- Lipomas (30%)
- Café-au-lait macules (9%)
- Acral and plantar keratoses
- Sebaceous hyperplasia
- Fibromas
- Haemangiomas
- Scrotal and furrowed tongue
- Neuromas
- Xanthomas
- Lentigines around the mouth, on hands, feet and genitals
- Vitiligo
- Acanthosis nigricans
Cowden disease
Bannayan-Riley-Ruvalcaba syndrome
The Bannayan-Riley-Ruvalcaba (BRR) syndrome is a rare germline mutation with hamartomatous polyposis, macrocephaly, and intellectual disability. Skin manifestations include:
- Genital lentigines, the most specific finding
- Facial papillomas
- Vascular malformations
- Lipomas
- Multiple acrochordons (skin tags)
- Acanthosis nigricans
Juvenile polyposis syndrome
Juvenile polyposis syndrome is a rare autosomal dominant disorder associated with hereditary haemorrhagic telangiectasia.
Neurofibromatosis
Neurofibromatosis is a common, autosomal dominant, a neurodermatosis characterised by:
- Café-au-lait macules
- Axillary and inguinal freckling
- Dermal neurofibromas
- Lisch nodules of the iris
- Systemic involvement, which can include gastrointestinal tumours
Neurofibromatosis
Cronkhite-Canada syndrome
Cronkhite-Canada syndrome is a sporadic syndrome that affects older adults. It presents with:
- Nail dystrophy (98%)
- Hair loss
- Diffuse hyperpigmentation
- Loss of taste
- Intestinal polyps
- Malabsorption
Paraneoplastic syndromes associated with gastrointestinal malignancies
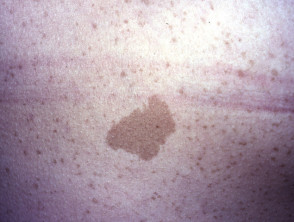
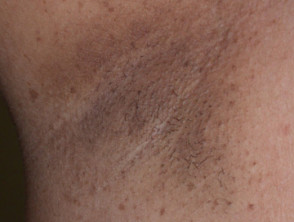
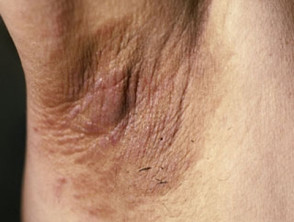
Acanthosis nigricans
Acanthosis nigricans is associated with insulin resistance.
- It is characterised by hyperpigmented, velvety, hyperkeratotic plaques.
- These affect axillary, inguinal, neck folds, mammary, umbilical and anogenital regions.
- In malignant disease, acanthosis nigricans can affect areola, digital web spaces, extensor sites and mucous membranes.
- Acanthosis nigricans associated with malignancy arises spontaneously and is rapidly progressive.
- Gastrointestinal adenocarcinoma can be responsible for acanthosis nigricans.
Acanthosis nigricans
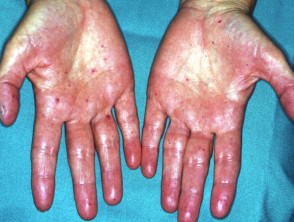
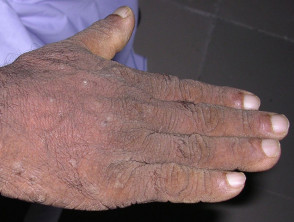
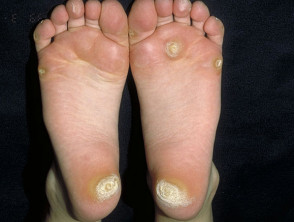
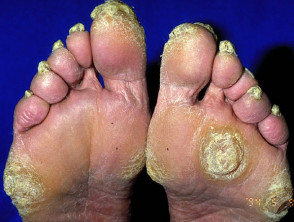
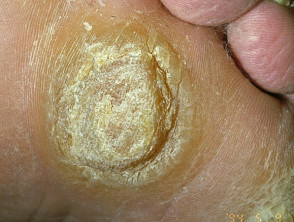
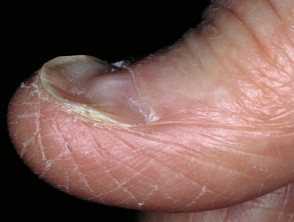
“Tripe palm” or palmoplantar keratoderma
Tripe palm is associated with malignant acanthosis nigricans.
- The abnormal palms are characterised by epidermal thickening with wrinkled broadened mesh-like ridges bounded by deep grooves within palms and fingers.
Tripe palms are associated with acanthosis nigricans
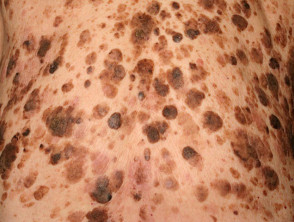
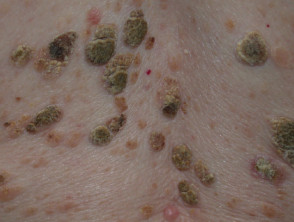
Multiple seborrhoeic keratoses
The acute onset of multiple, eruptive seborrhoeic keratosis is known as the sign of Leser-Trélat.
- Seborrhoeic keratoses initially erupt on the trunk, then on the extremities or face.
- When associated with gastrointestinal adenocarcinomas, the sign of Leser-Trélat carries a poor prognosis.
Seborrhoeic keratoses
Acrokeratosis neoplastica
Acrokeratosis neoplastica is also known as Bazex syndrome and is different from Bazex-Dupré-Christol syndrome associated with basal cell carcinomas.
- Acrokeratosis paraneoplastica is a rare, acral and psoriasiform dermatosis associated with cancers in upper respiratory and gastrointestinal tracts.
Glucagonoma syndrome
Glucagonoma is a rare, glucagon-secreting, pancreatic, alpha cell tumour.
- Glucagonoma is associated with necrolytic migratory erythema, a painful, pruritic, annular, erythematous eruption with central blisters, erosions, crusting and postinflammatory pigmentation.
Necrolytic migratory erythema due to glucagonoma
Tylosis
Tylosis is an autosomal dominant form of focal, non-frictional and nonepidermolytic, palmoplantar keratoderma.
- It involves more than 50% of the surface of palms and soles.
- Type A tylosis usually arises between 5 and 15 years of age; it is associated with oesophageal carcinoma at a later age.
- Type B arises in the first year of life and is generally benign.
Focal palmoplantar keratoderma (areata type)
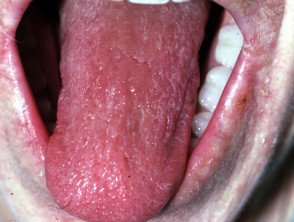
Plummer-Vinson syndrome
Plummer-Vinson syndrome is a rare triad of dysphagia, iron deficiency anaemia and oesophageal webs.
- Plummer-Vinson syndrome is associated with oesophageal squamous cell cancer.
- Skin signs include:
- Brittle koilonychia (spoon-shaped, thin nail plates)
- Oral leukoplakia due to intraepithelial carcinoma
- Angular cheilitis
- Pale, atrophic buccal mucosa
- Glossitis
Iron deficiency
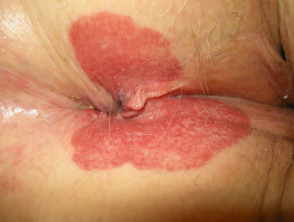
Extramammary Paget disease
Extramammary Paget disease is an intraepithelial adenocarcinoma located in and around the anal verge, vulva, or male genitalia.
- Anal Paget disease is associated with anorectal adenocarcinoma.
- It presents with a slowly-enlarging, unilateral, dry, scaly plaque.
Perianal extramammary Paget disease
Carcinoid syndrome
Carcinoid syndrome is the association of intestinal carcinoid with hepatic metastases.
- Carcinoid syndrome causes flushing and diarrhoea.
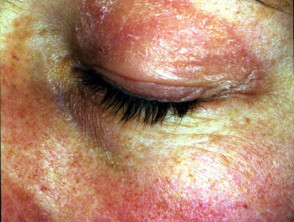
Dermatomyositis
Dermatomyositis is classified as an autoimmune disease. In older adults with dermatomyositis, 15–50% have an underlying malignancy of the gastrointestinal tract, pancreas, lung, breast, or ovaries, or non-Hodgkin lymphoma.
- Dermatomyositis associated with malignancy may precede the diagnosis of cancer by about six months.
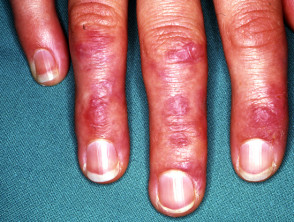
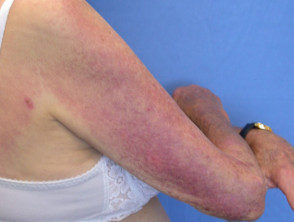
- Skin signs of paraneoplastic dermatomyositis include:
- Heliotrope rash with periorbital oedema
- Gottron papules on finger joints
- Violaceous poikiloderma over the chest, upper back, elbows and knees
- Nail signs: “ragged cuticle” and nail fold telangiectasias.
Dermatomyositis
Paraneoplastic pemphigus
Paraneoplastic pemphigus (PNP) is a rare acantholytic, mucocutaneous blistering disease.
- PNP is rarely associated with tumours of the gastrointestinal tract.
- Other associated cancers include non-Hodgkin lymphoma and other haematological diseases, thymoma, sarcoma, lung cancer, and melanoma.